In This Article
By now you have certainly heard of coronavirus in the news. From the media reports, you would think we should be prepared for the end of days. But should we? We first need to understand what the virus is and what to expect from it. We should also compare it to some other outbreaks of viruses as well.
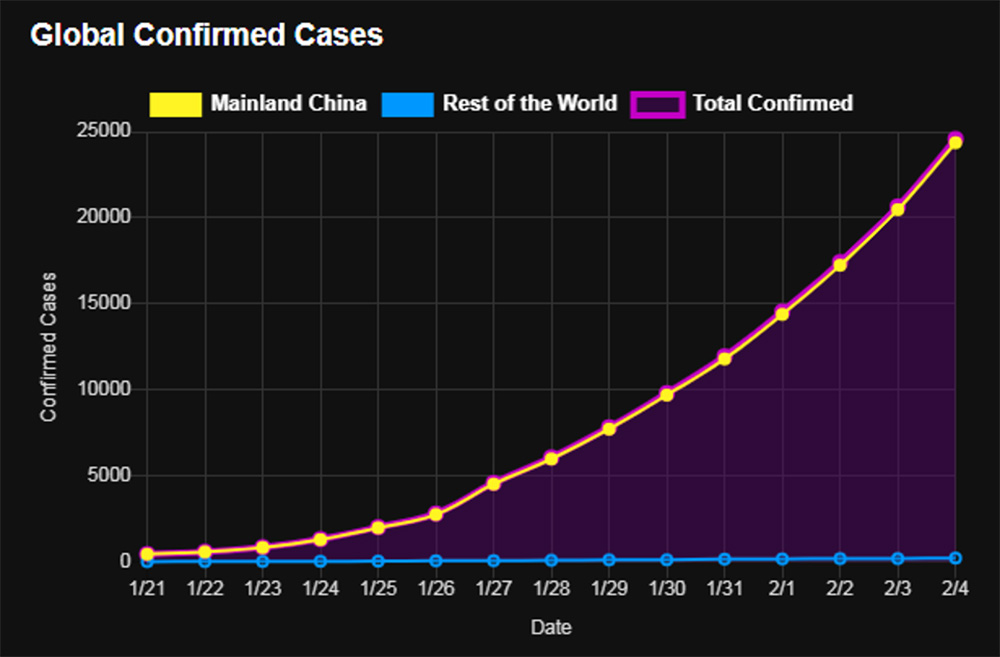
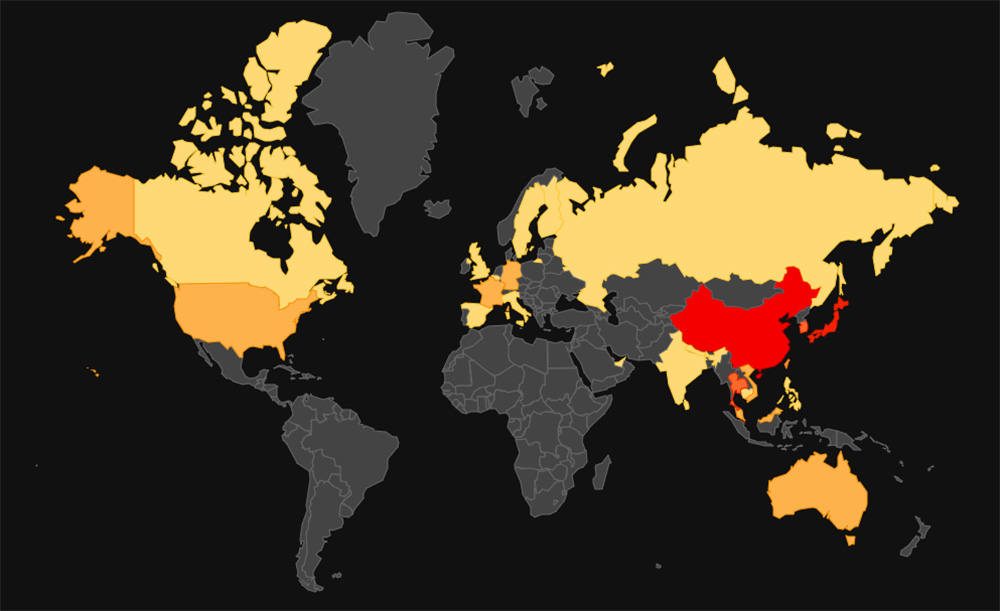
Currently, there are seven strains of coronavirus that infect humans. The newest is the novel coronavirus (nCoV). It is similar to a different coronavirus that has caused the Middle East Respiratory Syndrome (MERS –CoV), which has been sporadic in northwest Africa since 2012. This MERS – CoV infected nearly 2,500 people worldwide in 2019. As for the new nCoV, as of February 4, 2020, there have been 20,630 cases reported worldwide with 23 countries reporting cases. In the United States there have been twelve reported cases (as of Feb. 5), according to the World Health Organization. Eight of the cases in the US have been associated with travel from China, two from person to person contact within the US and two more that have yet to be classified. These cases have occurred in California (six cases), Illinois (two), Washington (one), Arizona (one), Massachusetts (one) and Wisconsin (one).
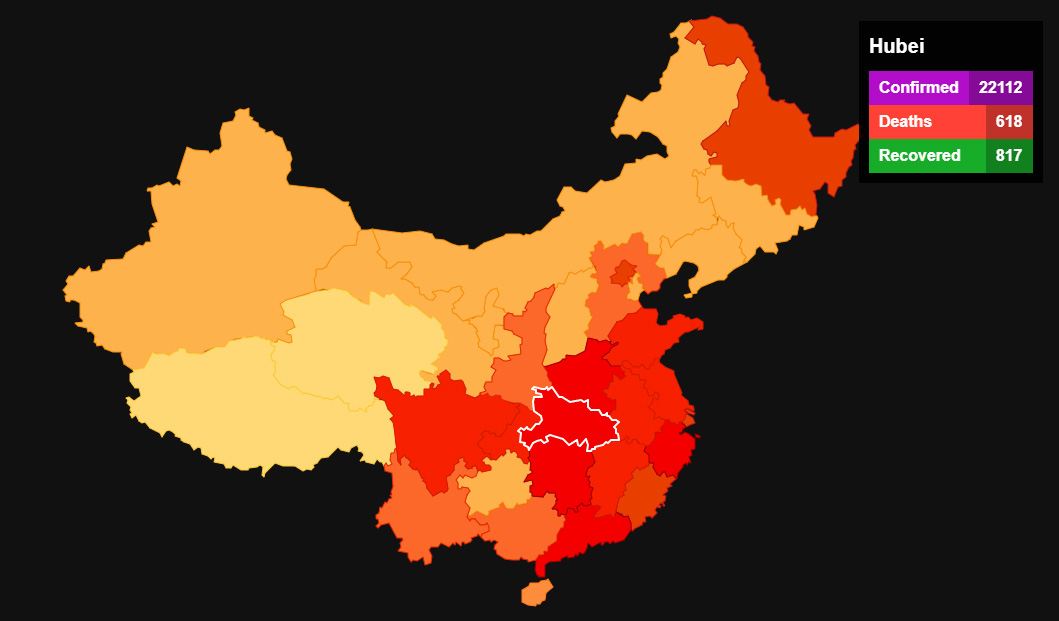
This particular novel coronavirus (nCoV) started in Wuhan, China and has been named the Wuhan Flu. It just so happened to have its epicenter near a lab that studies the virus.
Although reports suggest animal to person contact from a market in Wuhan, my suspicion is that there was probably a breach of protocol in that lab where someone became contaminated and allowed the virus to spread to other people. The reason it is called a ‘novel’ coronavirus is that it is a little different genetically than previous coronaviruses and had not previously been found to infect humans. Typically, the coronavirus is seen in animals and infrequently spreads to humans. When it infects humans, its symptoms and severity are worse than the typical influenza virus.
Symptoms
Once a human is exposed, symptoms can begin in 2 – 10 days with a mean of 5 days. Symptoms may include fever, cough, and significant shortness of breath, along with fatigue, muscle aches, and headache. Watery diarrhea may also be present. The shortness of breath can be progressive through the course and the diarrhea, if present, usually appears in week two of the illness. People who are at risk of infection are those people in close contact with those infected, as well as those with chronic diseases (e.g., diabetes, chronic kidney disease, chronic lung disease, and immunocompromised patients). The contagious period is most likely in the second week of illness.
Treatment
There is no specific treatment for the virus and care is supportive in nature. Hospitalization may be needed for administration of fluids for dehydration and supplemental oxygen for the shortness of breath. Acetaminophen can be given for the fever. Presence of concomitant diseases (mentioned above) also increases the risk of hospitalization. Of course, the patient should get as much rest as possible to allow the body to heal. Symptoms can last two weeks with recovery following according to the severity of disease.
How Contagious Is It?
Regarding contagion, there is a mathematical term called R0, or R naught. This reflects the relative contagious capacity of infectious disease. If a disease has a R0 value of 1.0, this reflects that for every person infected, they will spread it to one other person. Influenza’s value is 1.28. MERS was reported to be less than one while SARS was estimated to be between 2 – 3. This Wuhan Flu is thought to have a R0 of 1.5 – 3.5 with some suggesting the upper limits of that range. Keep in mind that a value of less than one will cause the outbreak to diminish. Ways that public health can control the spread is to limit travel to endemic areas as well as to quarantine those travelling. We have already seen flights being limited to and from China as well as two cruise ships being quarantined due to case reports of Wuhan Flu on board the cruise ships.
Detecting the Virus
With the timing of this outbreak, in the midst of flu season, how do you know if you have influenza versus coronavirus?
Initially, you may not know the difference, as some of the symptoms overlap. As the shortness of breath progresses during the first week, it may require a visit to the doctor. But keep in mind that you should wear your N95 mask and take precautions as if you ARE infected. There is a test that can be done for flu in most physicians’ offices and in hospital labs to test for influenza; however, testing for the nCoV is only done by the Centers for Disease Control at present. The CDC is working on releasing the protocol to test on a more widespread basis. Another factor to distinguish between the two viruses is whether you have traveled to an area that has reported cases of the nCoV or have come in contact with someone who has tested positive. Last, if you were diligent in getting your flu shot this year, this will likely reduce your severity of illness due to the influenza virus. Although that vaccine has no impact on whether you catch coronavirus, it may help health officials decide how to distinguish between the two in the early phases.
Comparing the Mortality Rate
So why should we care if it’s the flu or coronavirus?
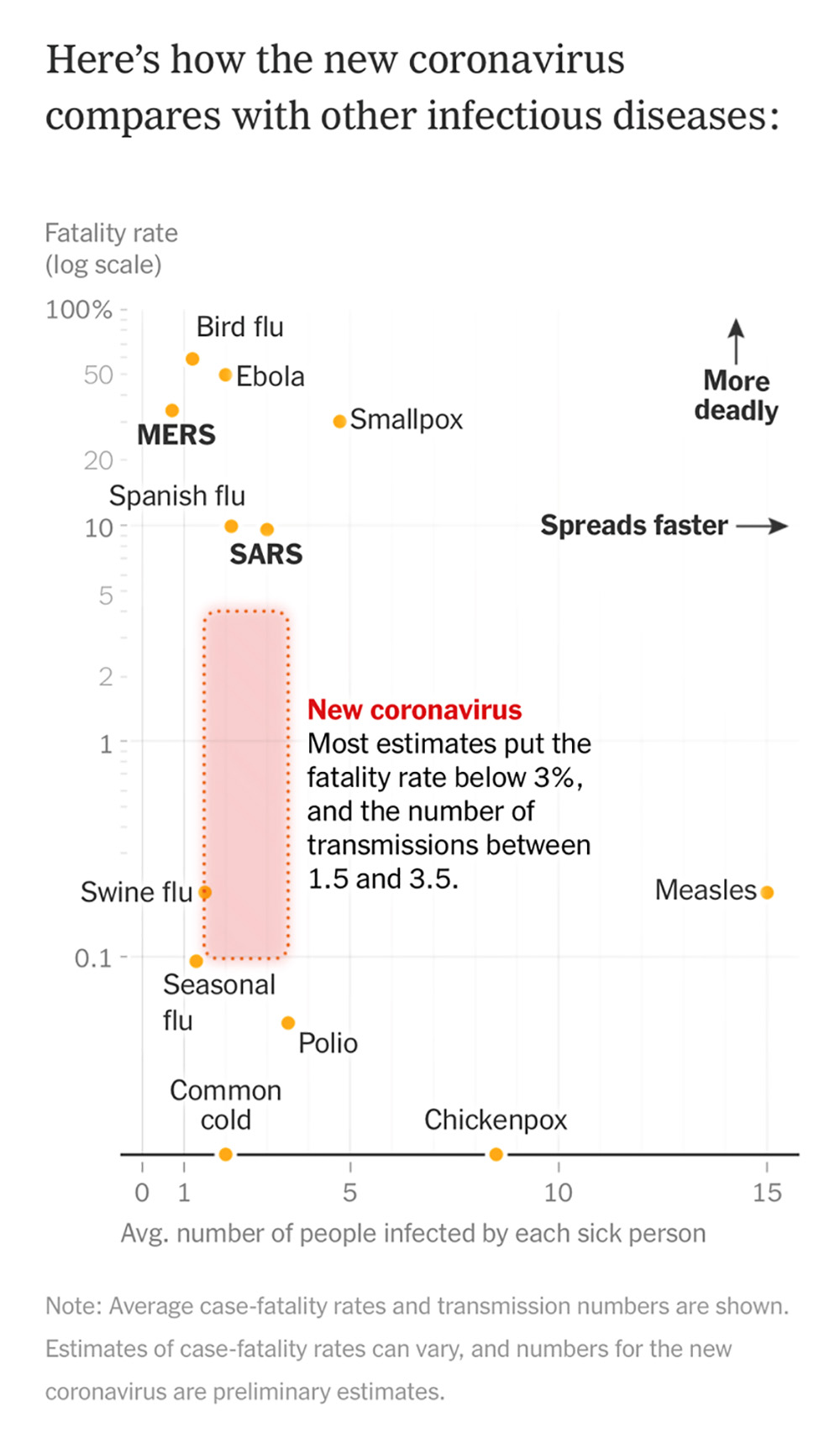
From what has been observed to date, this novel coronavirus kills about 3% of those infected. This is compared to about 0.01% of those affected by influenza. Keep in mind this percentage of nCoV is potentially an early underestimation of mortality while the number of total cases rises exponentially. It will only be after the dust settles that we truly know what the mortality was with this disease. And, while 3% doesn’t sound like much, it is certainly more deadly and more contagious than the flu.
Above: This graphic from The New York Times compares the fatality rate and contagious capacity of the Novel Coronavirus.
In addition, the number of severe complications for Wuhan flu is reported to be in the 20 – 30% range. These persons will spend time in the intensive care unit of the hospital and have prolonged hospitalizations as well. And as far as the two other coronaviruses mentioned above, in 2003, Severe Acute Respiratory Syndrome, or SARS –CoV, which was thought to have come from the Chinese civet cat, had a mortality of about 10%, and the Middle East Respiratory Syndrome (MERS –CoV) had a mortality of 35%. (This appeared as recently as last year in Saudi Arabia and was thought to be transmitted initially from camels.) Both of these two latter viruses had R0 factors less than what the nCoV show so far.
Because there are no vaccines for coronavirus, the Centers for Disease Control and the World Health Organization recommend avoiding crowds, frequent handwashing, wearing masks (N95 preferably) while in public, avoiding touching eyes, nose, or mouth, and using disinfectants or hand sanitizers. Common sense should also encourage you to stay home when sick.
Conclusion
From a public health perspective, this Wuhan Flu is potentially 3 – 4 times more contagious than the influenza virus and three times more likely to result in death. The World Health Organization declared the Wuhan Flu to be a global health emergency and, along with the Centers for Disease Control, is taking significant measures to limit the spread of the virus outside of China. Personal responsibility to limit your exposure should also come into play. Stay home if you are sick. Wash your hands frequently. Cover your mouth when you cough.
Anytime a new kid comes to town, or a new infectious disease, it gets people excited. This particular novel coronavirus is of interest because it has the potential, if it gets out of control, to have significant health and even economic impact globally (watch George Gammon’s YouTube video for more details).
We are all familiar with influenza and are too often blasé about its impact on our lives. But we have faith in our influenza vaccines and our ability to recover from influenza. Think about your chances of recovery if you contracted the Wuhan Flu, though. You may feel horrible for two weeks and be on the mend. Or you could be one of the 20% who end up in the intensive care unit and on a ventilator. Or you could be one of the 3% who die. So, should we be concerned? While a 3% chance of death doesn’t sound like much, in medicine, it’s more risk than we like to see.
About the Author
David L. Miller, DO FACOI, is an internist in private practice for 20 years. His experiences away from the office have included time as a fight doctor in regional MMA events and as a team physician for 10 years at a mid-major university in the Midwest. Currently, he serves as the lead medical instructor for the Civilian Crisis Response team based out of Indianapolis.