In This Article
This article originally appeared in Issue 3 of our magazine.
WARNING: This article is meant to be a quick overview and not a detailed guide on procedures relating to the treatment of burns. To be prepared for any emergency, we encourage you to enroll in a certified medical course or, at a minimum, a familiarization course, which will deliver comprehensive knowledge of how to treat different types of burns.
When early mankind discovered fire and its many wonderful uses, mankind surely also quickly became aware of one of its painful consequences — burns. Though we have evolved since then, some more than others, modern man continues to deal with burn injuries and treatments. Most burns are caused by thermal heat, which we will discuss further, but some are due to a chemical or an electrical source.
First Action
The first action to take is to move the burnt area away from the heat source, and measures must be taken to stop any residual flames. Remember your schoolyard teachings…no, not “don’t eat glue,” but rather “stop, drop, and roll.” Second, assess the damage in terms of location, extent, and degree of the burn.
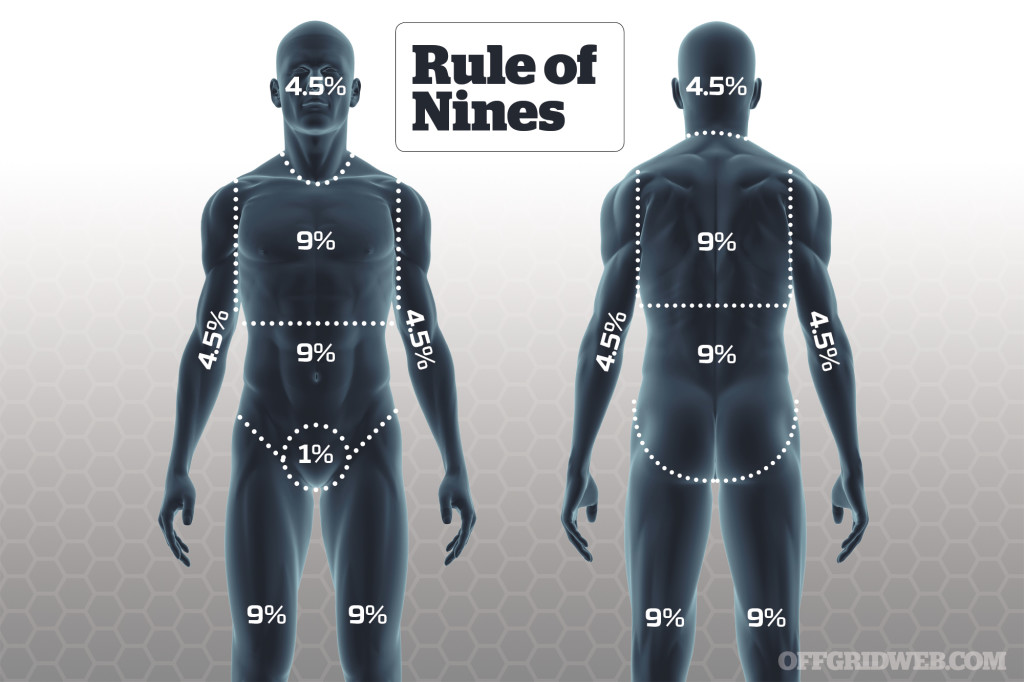
TBSA and the Rule of Nines
You can determine the extent of the damage in terms of Total Body Surface Area (TBSA) by using the “palmar method” and the “rule of nines.” The area of a victim’s palm is considered to be equivalent to 1 percent of TBSA. The “rule of nines” estimates the surface area of each main body part in multiples of nine (see diagram).
Since burns are never uniform, a quick estimate can be made by combining the two rules. Using the palmar method, if a victim has a burn the size of three of their palms on their leg, you can estimate that they have a burn on 3 percent of their body. If one entire arm has burns on it, a quick assessment using the rule of nines would conclude that the victim has 9 percent of their body burnt. If one leg was completely burnt, that would represent 18 percent.
Classifications
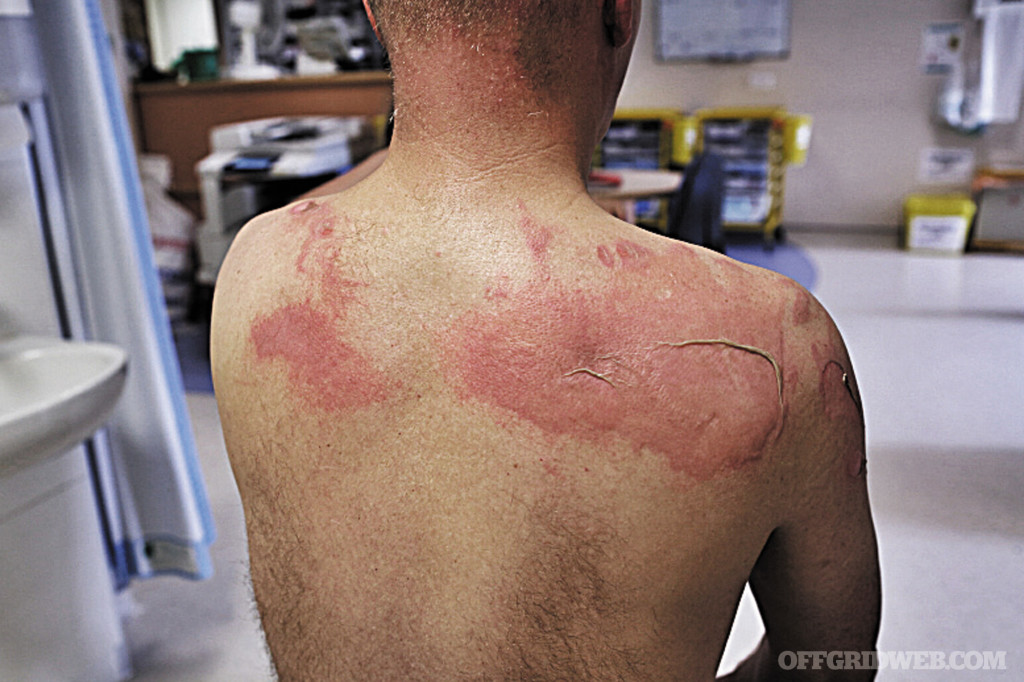
Burn classifications — first-, second-, or third-degree — can be used to assess the severity of the injury. The majority of burns are first degree, which affect the outer layer of skin, causing redness, light pain, and some swelling. Symptoms are similar for second-degree burns, which also have additional blister formations at the burn site. Serious second- and third-degree burns are discussed later in this article.
First Degree (Superficial)
Layers Affected: Epidermis
Appearance: Redness
Texture: Dry
Healing Time: 2-10 days
Complications: Increase of skin cancer, typically no scarring
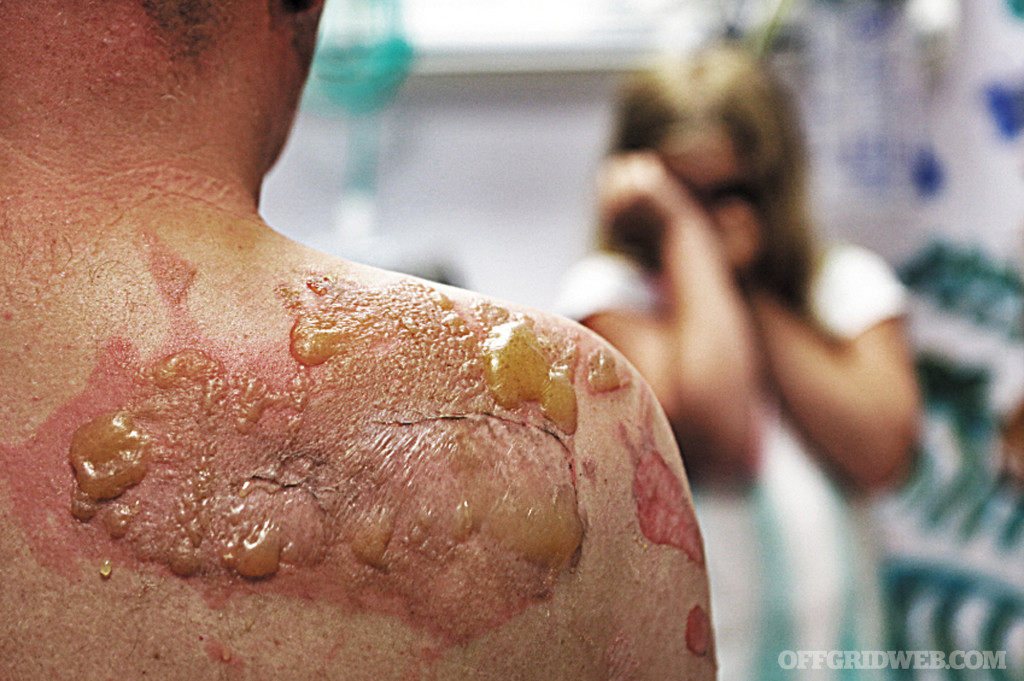
Second Degree (Superficial Partial Thickness)
Layers Affected: Extends into superficial dermis
Appearance: Redness with clear blister
Texture: Moist
Healing Time: Less than 2-3 weeks
Complications: Local infection, typically no scarring
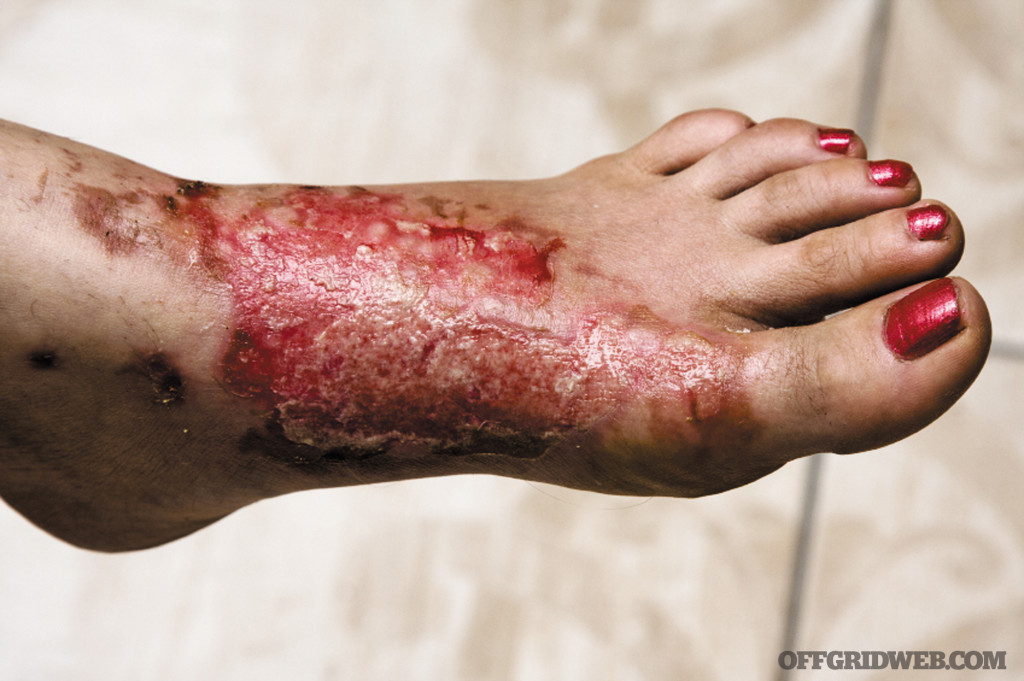
Second Degree (Deep Partial Thickness)
Layers Affected: Extends into deep dermis
Appearance: Red with white and bloody blisters
Texture: Mostly dry
Healing Time: 3-8 weeks depending on severity
Complications: Scarring, contractures (hardening of tissue), possible skin grafting
Third Degree (Full Thickness)
Layers Affected: Extends through entire dermis
Appearance: Stiff, white/brown
Texture: Tough, leathery
Healing Time: Months
Complications: Scarring, contractures (hardening of tissue), possible amputation
Fourth Degree
Layers Affected: Extends completely through to muscle and bone
Appearance: Black, charred
Texture: Dry
Healing Time: Little to no chance of recovery
Complications: Amputation, loss of function, possible death
Treatment
Treatment for first-degree and small second-degree burns (less than 3-4 inches in size) involves running cold water or placing a cool compress over the injury for 10-20 minutes. Never directly apply ice on the wound — several studies have shown this may constrict local blood vessels, which may lead to further damage to the affected tissue. Though blisters may be painful, do not attempt to pop them because open blisters reduce healing time and are magnets for infections.
Immediately after cooling, gently wash loose debris from the area, dry it off, and dress the wound loosely with any available clean gauze or clothing. When possible, wash and redress the wound twice a day. If a clean dressing is not available, do not apply anything to the burn, but rather allow the area to form a dry hardened layer, which is your body’s own natural protection.
Topical antibiotics can be applied to the wound to prevent infection. It is important to remember the advice of your cardiologist, “hold off on the butter.” Contrary to popular belief, butter is not a wise treatment and can lead to delay in recovery. Of all the home remedies, applying honey on the wound has some street cred because many studies have shown it effectively improves healing time and prevents infection. Most first-degree burns will heal completely within a week, while second-degree burns take two to eight weeks with some scarring.
Serious Burns
Deep second-degree burns covering more than 10 percent TBSA and third-degree burns are a whole ’nother beast when it comes to treatment, because you will also need to address problems that are not located at the burn site. First, it is important to check breathing and blood circulation. If needed, perform CPR.
Never treat large body areas with cold water because this can cause both hypothermia (drop in body temperature) and traumatic shock (drop in blood pressure and circulation). To prevent hypothermia, wrap the victim in a blanket or any other covering. In case of shock, have the victim lie down on their back, then elevate and support both legs and arms up high above the heart to keep blood flow near the center of the body.
Clothing, or any other object, can get lodged into the burn area due to the high amount of heat. Do not attempt to forcibly remove these objects, as this may cause additional tissue damage and possible bleeding problems. Loose clothing around the lodged material can be carefully cut away.
Third-degree burns can turn the skin ash white, brown, black, or gray with charring effects. Due to the extreme damage to the skin, pain may be actually be absent and blisters will not form at the site. For mild third-degree burns and those covering less than 5 percent TBSA, the burn area can be treated like first- and second-degree burns.
Head and Neck
Serious second- and third-degree burns or major burns to the head area will require a rapid response by medical experts. Once the victim is fully stabilized, immediately execute an evacuation plan to get the victim to a trained professional. Some burns involve the inhalation of hot fumes that can damage the respiratory tract. Burns around the face and neck or burnt debris in the nasal and mouth cavity may signal airway damage, which will also require immediate evacuation.
Play it safe and seek trained help when in doubt. In the worst-case scenario where help is not available, keep the victim calm and stable while continuing to monitor their vitals, breathing, circulation, hydration, and body temperature. Preventing infection is crucial, so oral antibiotics can be administered, if available. Allow the victim to rest, while giving them time to recover from the traumatic ordeal.
In all burn cases, stay calm, but react quickly while paying attention to how the victim responds. Whether smoking while using hairspray or sipping a bit too much moonshine around a campfire, be careful. But when the time comes, treating burns correctly will ensure proper healing and prevent life-threatening situations.