In This Article
Disclaimer: This article about improvised antiseptics is meant to be a brief overview and not a detailed guide on treating or preventing infection. Always seek professional medical help before attempting any of the steps outlined in this article.
In good times or bad, families may face any number of events where trauma causes injuries. In the United States alone, there are over 37-million emergency department visits annually due to injuries. Off the grid, activities of daily survival performed by those unaccustomed will greatly increase the number of traumatic wounds. In austere settings, many of these become infected. Failure to act can only lead to headaches (and heartaches) for the family caregiver.

What is an Antiseptic?
Antiseptics (from the Greek anti “against” and septikos “rotting”) greatly decrease the number of disease-causing organisms on skin and mucous membranes. Having antiseptics on hand can save lives, but your supplies will eventually run out in a long-term disaster. In this article, we’ll discuss how to use antiseptics as well as how to improvise germ-killing agents off the grid.

Many people confuse antiseptics, disinfectants, and antibiotics. The goal of all of these substances is to combat infection, but they’re not the same. Disinfectants are applied to nonliving surfaces, such as countertops or tubs. Antiseptics, on the other hand, are applied to the surfaces of living tissues. Doctors apply disinfectants to clean their exam table, then use antiseptics on the skin of patients undergoing procedures on that table. Antibiotics are most commonly ingested by or injected into a patient, something you don’t want to do with either disinfectants or antiseptics.
Above: Boiling water eliminates enough microbes to allow it to be used in wound care.
Ways Antiseptics Can Prevent Infection
Antiseptics are useful for…
Cleaning hands: Antiseptics are commonly included in scrubbing before exams, surgery, and other medical procedures.
Mucous membranes: Mucous membranes include the oral and nasal cavity, vagina, and urethra. They can be utilized to prevent or treat infections, such as before inserting a urinary catheter or as antiseptic lozenges to help with bacterial throat infections.
Prepping skin before procedures: When applied to the skin, certain antiseptics protect against the invasion of microbes into surgical incisions or other open wounds.
There’s some controversy as to how effective antiseptics are when used on open wounds, due to some being somewhat toxic to new cells. Many, however, are helpful if used properly.
Commercial Antiseptics
Various types of commercial antiseptics exist. Two of the most popular are povidone-iodine (Betadine) and chlorhexidine (Hibiclens), which also are available as oral rinses. These products are used by caregivers to scrub hands and “paint” areas on the body where incisions are made. Also, compounds containing silver have been used to keep wounds free of infection.

Povidone-iodine: Betadine, when diluted with saline solution, decreased infection rates when flushed in wounds associated with hip and knee procedures. For skin, gently clean the affected area with soap and water. Apply Betadine to the affected area during wound care; let dry before bandaging. A 2×1-inch wipe contains about 10 drops of povidone-iodine. Not for use in people with hyperthyroidism or recently exposed to radioiodine.
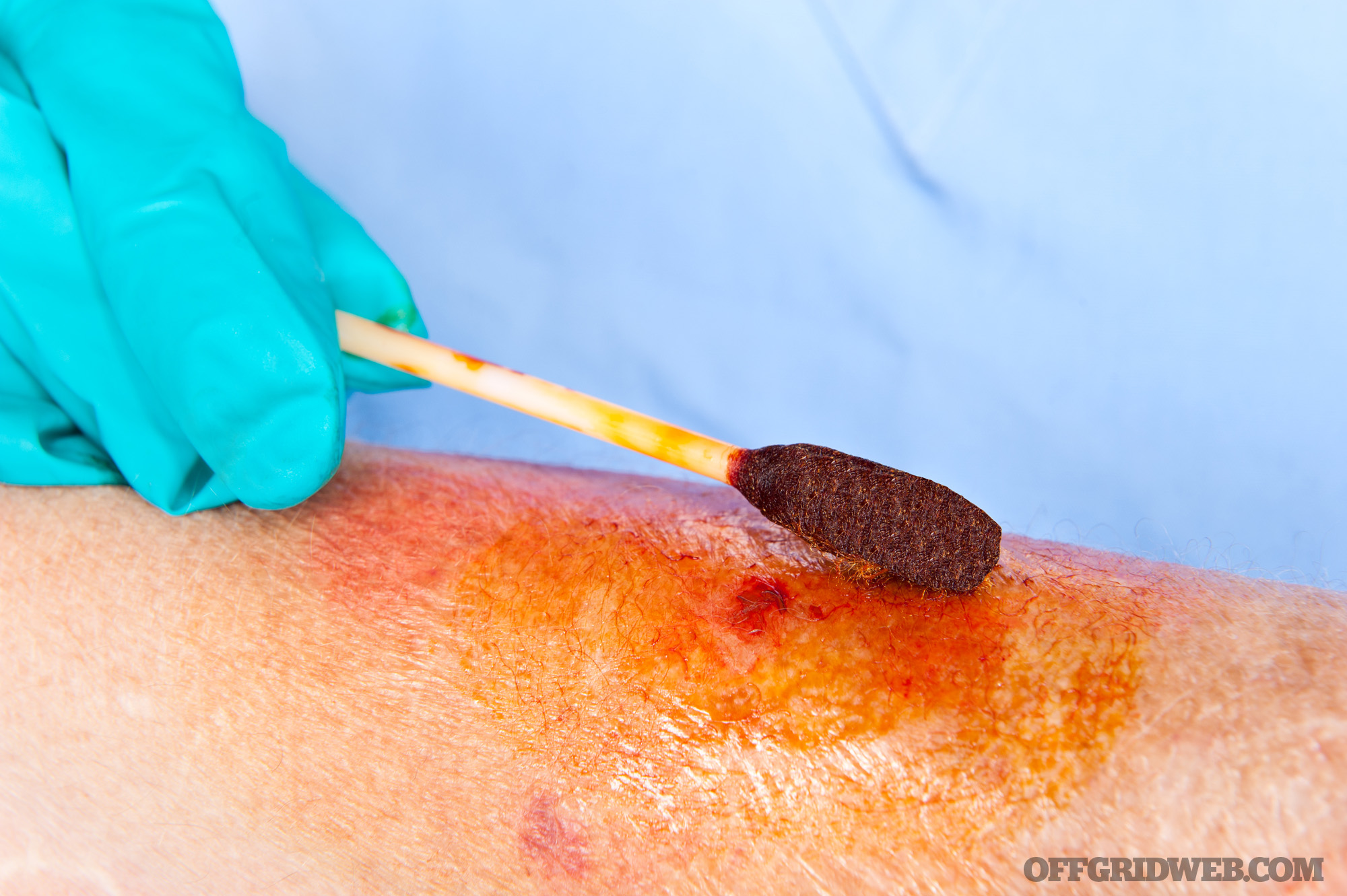
Chlorhexidine: Considered to be superior to povidone-iodine as an antiseptic prior to performing surgical procedures, chlorhexidine is usually applied to unbroken skin or small, shallow cuts. It’s not meant for use in deep lacerations or other open wounds.
Silver compounds: Although not used for surgical procedures, topical silver solutions were thought to be effective against various types of wounds. Indeed, before there were antibiotics, silver compounds were applied to skin lesions. Drinking silver ionic solutions, however, is more controversial as to its effectiveness against infections.
Household Products as Improvised Antiseptics

Many household products are also known for their antiseptic properties. Sodium hypochlorite (household bleach), hydrogen peroxide, alcohols, and others have been used for more than a century to prevent and fight infections.
Chlorine products: Germ-killing solutions can be made from liquid bleach (sodium hypochlorite) or solid crystals (calcium hypochlorite). Often used as a disinfectant on surfaces, it can, if used properly, also be helpful for wound healing.
Although not commonly used today, a sodium hypochlorite solution in varying concentrations was a standard wound cleaning solution during World War I. Known as Dakin’s solution, it’s simply a warm mixture of bleach, baking soda, and boiled tap water. Be aware that the strongest versions are used for infected areas and should only be used off the grid in severe cases.
DAKIN’S SOLUTION RECIPE
| Ingredient | Full Strength | 1/2 Strength | 1/4 Strength |
|---|---|---|---|
| Bleach | 6tbsp (or 95ml) | 3tbsp + 1/2 tsp (or 48ml) | 1tbsp + 2tsp (or 24ml) |
| Water | 32oz or 1 liter | 32oz or 1 liter | 32oz or 1 liter |
Calcium hypochlorite: Available as crystals in certain pool-cleaning products. To make a chlorine solution with calcium hypochlorite, add 1 heaping teaspoon to 2 gallons of water and stir. This makes a “bleach” that can be used to make Dakin’s solution or to disinfect drinking water. For drinking water, use eight drops per gallon; double the dose if the water is cloudy, colored, or very cold. Wait a full 30 minutes before using. Although crystalline calcium crystals store well, bleach in solution will lose potency after six to 12 months.
Hydrogen peroxide: A 1:1 mixture of hydrogen peroxide and water has been used as an antiseptic mouth rinse with some success. It’s not safe, however, to swallow. Although it has been used on open wounds as well, newly formed cells love moisture and may not tolerate the drying effect of hydrogen peroxide. As such, it’s generally discouraged for wound care.
Isopropyl alcohol: Isopropyl (rubbing) alcohol is best used on intact skin, scratches, and shallow cuts, but is excessively drying to apply to large open wounds. The alcohol percentage in the product should be in the 60- to 70-percent range to kill microbes. Such is the case with hand sanitizers. You might be surprised to learn that this fact makes alcoholic beverages less than effective as an antiseptic. Eighty-proof vodka, for example, is only 40 percent alcohol!
Plant-Based and Other Natural Antiseptics
When the commercial antiseptic products run out, the family medic will need to look to nature for substances that can prevent and treat infection. Some plant extracts are thought to have significant antiseptic properties:
Honey: Applied to open wounds full strength or diluted with water, raw unprocessed honey has been found to prevent growth of many species of bacteria. Its pH profile promotes oxygen delivery to wounds. Some researchers believe raw honey to be superior to antibiotics in treating certain drug-resistant bacteria. Commonly used for bites, stings, cuts, burns, and infections.

When using raw honey on wounds, always start with clean hands and, if possible, sterile dressings. To avoid a messy proposition, put the honey on the dressing before applying to the wound. An exception would be a large, deep wound. In that case, fill the wound with honey before placing a dry dressing. Be aware: There will be seepage, so cover well. Replace when wound drainage saturates the dressings. It should be noted that there are commercially made honey-impregnated dressings available (MediHoney).
Tea tree oil: A well-known natural antibiotic, this pungent oil contains antiseptic compounds that are effective against fungal infections like ringworm, athlete’s foot, and jock itch as well as wound healing. For wound cleansing, add 1½ tablespoons of tea tree oil to a cup of warm water.
Turmeric paste: A compound in turmeric called curcumin possesses antimicrobial properties, which may enhance wound healing. Mixing turmeric and warm water to make a paste has been used to successfully treat dry socket, a common infection that occurs after removing a tooth. Apply the paste gently and cover with a small amount of gauze.
Witch hazel: This is a mild antiseptic with astringent property. Largely used for acne these days, it can serve as a gargle for throat issues or can be applied directly to mild wounds.
Aloe vera: A member of the cactus family, aloe vera contains a gel-like substance called glucomannan that promotes wound healing. Aloe vera is a popular natural treatment for burn injuries as well. Apply a thin layer or wet a bandage with it and cover the wound.
Coconut oil: Coconut oil contains monolaurin, a fatty acid thought to have antimicrobial effects. It can be used as a base to make antiseptic ointments.
Garlic: Garlic is well-known for antimicrobial properties due to a substance it contains called allicin. One study using an ointment containing garlic showed better wound healing than Vaseline. Simply crush a clove of garlic and mix it with a third of a cup of water or some coconut oil. Use the product right away, as it loses potency in just a few hours.
Salt: Although sea water is risky to use as an antiseptic, flushing a wound with sterile salt (“normal saline”) solutions is thought by some to decrease the risk of infection. Mix a liter of water and 2 teaspoons of salt in a pot with a lid and boil for 15 minutes. Let cool and use immediately or seal in sterile canning jars. Interestingly, some studies have found that drinkable tap water may be just as effective.
Vinegar: Standard white vinegar contains 4- to 7-percent acetic acid and 93- to 96-percent water. Mildly effective against certain disease-causing microbes that infect, for example, burn wounds, apply at least twice a day.

There are many other natural substances that have had antiseptic properties attributed to them, including the following:
- Anise oil
- Lavender oil
- Eucalyptus oil
- Baking soda
- Camphor
- Cinnamon oil
- Citronella oil
- Frankincense oil
- Myrrh oil
- Lemon juice or oil
- Oregano oil
- Spearmint oil
- Sweet orange oil
It’s important to realize that the evidence for the antiseptic effects of many natural substances is limited in terms of hard scientific data. They also are difficult to standardize in any meaningful way and, thus, different versions of the same substance may vary in their effect on different individuals. There’s also the possibility of allergic reactions. Do your own research and make your own conclusions.
What About Soap?
Regular soap isn’t technically an antiseptic because it doesn’t kill bacteria. So, why use soap and water to clean wounds? Soap lather causes microbes to be more easily rinsed away with the stream of water. More bacteria will be dislodged the longer you scrub, but they remain alive even as they go down the drain. Certain soaps contain antibacterial agents, but they’ve been found to not be very effective, could possibly cause reactions, and may contribute to the ongoing epidemic of antibiotic resistance. Therefore, some have been removed from the market.
Does Salt in a Wound Really Help?
In centuries past, punishment for sailors at sea involved lashes with a whip. Since these whippings broke the skin, salt or saltwater was rubbed into the wound to (in theory) prevent infection. But just because salt was used historically as an antiseptic, doesn’t mean it really worked. Researchers have since found that rinsing a wound in seawater is harmful due to the presence of dangerous marine microbes. Additionally, many bacteria tolerate salt very well, including the organism behind deadly MRSA infections. Therefore, the saying “rubbing salt in the wound” became a metaphor for making a bad situation worse!
A Veterinary Alternative
A combination of commercial and natural antiseptic products known as sugardine (or sugardyne) is an additional option. Various studies have shown the mixture of sugar and povidone-iodine is effective for wound management. It appears that sugardine nourishes regenerating tissues and inhibits the growth of bacteria.
Several formulas have been published, depending on the thickness of the paste desired. It appears like thick honey in concentrated form (9:1 sugar: povidone-iodine) and less viscous when more dilute (as low as 2:1). An alternative to povidone-iodine is hydrogen peroxide, which seems to be less toxic to healing cells when a large amount of sugar is added. No approved standard exists with any of these combinations. Be aware that sugardine can get stiff in cold weather.
With a little knowledge and imagination, improvised antiseptics can help the family medic decrease the risk of infection, furthering the goal of keeping people healthy, even when off the grid.
About the Author
Joe Alton, MD, is a physician, medical preparedness advocate, Life Fellow of the American College of OB/GYN, retired Fellow of the American College of Surgeons, and member of the Wilderness Medical Society. He’s the NY Times/Amazon bestselling author of the Book Excellence Award winners in Medicine: The Survival Medicine Handbook and Alton’s Antibiotics and Infectious Disease as well as several other books. He’s also founder of the award-winning survival website DoomandBloom.net and designer of an entire line of quality medical kits at store.doomandbloom.net.






