In This Article
Imagine grabbing a searing-hot pan straight out of the oven. The pain hits you in a split-second, and you jerk your hand away in shock, cursing under your breath as you run your fingers under cool water to soothe the throbbing. The skin becomes red and inflamed, and eventually forms a fluid-filled blister. Eventually, the blister will drain, and the wound will scab over. Permanent scarring may also occur. It’s an extremely unpleasant experience, to say the least.

Most of us have been burned at one time or another, leading to an extra level of caution when dealing with extreme heat. However, many Americans are not adequately prepared for the severity of injuries that may occur at the opposite end of the temperature spectrum. Tissue and skin injury from extreme cold is known as frostbite, and its symptoms can be just as destructive as serious burns.
In fact, frostbite may pose an even more insidious threat, since its numbing chill lulls victims into a false sense of security. While it can cause tissue damage and blistering similar to a burn, frostbite won’t necessarily produce the instant pain response like our example of grabbing a hot pan. If you’re unprepared and unaware of the initial warning signs of frostbite, you or someone you know may fall victim to this dangerous condition this winter.
To adequately defend against frostbite, there are three key points to consider. First, we must diagnose the signs and symptoms of its onset. Second, we need to know how to treat frostbite, and alleviate the damage and pain it causes. Finally, we should prepare ourselves with the gear and mindset to prevent frostbite in the first place. Follow along as we address each of these points below.
Diagnosis

Frostbite is a direct byproduct of the human body’s natural reaction to extreme cold. In order to preserve its core temperature and protect the vital organs, the body forces blood vessels near the skin’s surface to constrict. This consolidates warm blood closer to the core, delaying the onset of hypothermia and keeping you alive. However, it also begins to starve your extremities of blood flow and warmth.
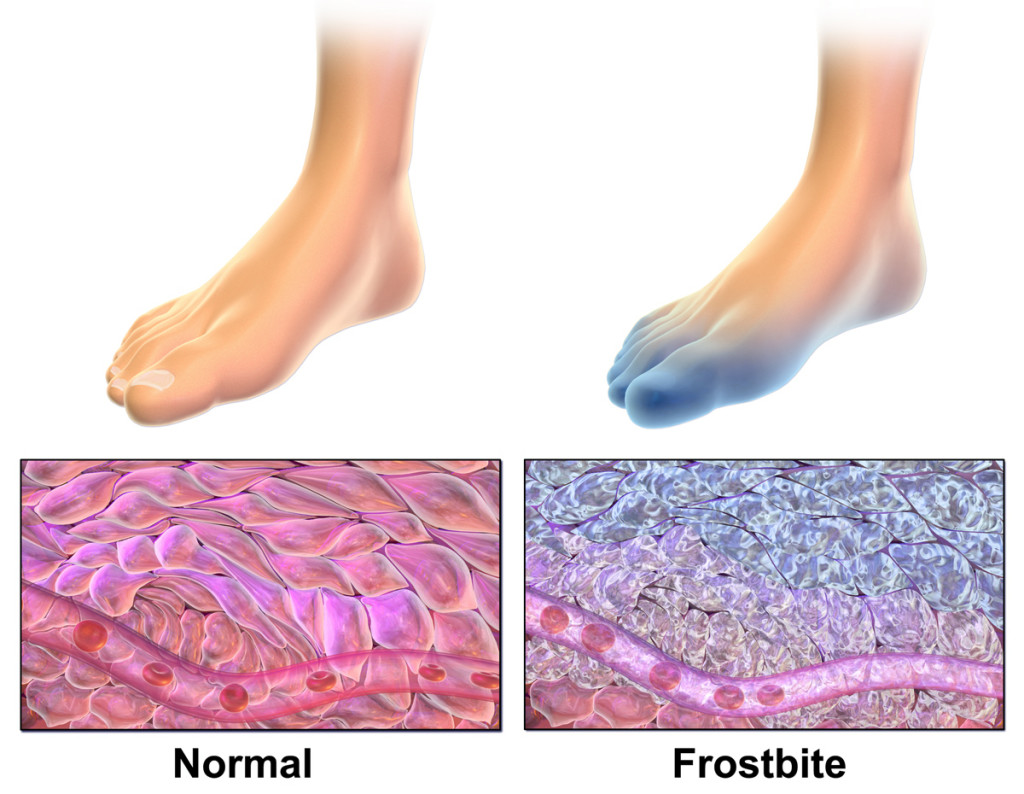
The University of Maryland Medical Center explains the biological mechanism:
“At first, the blood vessels alternate between narrowing and widening, to keep the extremities as warm as possible. But under extremely cold conditions, the vessels stop widening. When skin temperature drops low enough, ice crystals can form around and within the cells, freezing tissue and possibly rupturing cells. The lack of circulation that occurs when the body directs blood flow away from the extremities may also cause cell damage.”
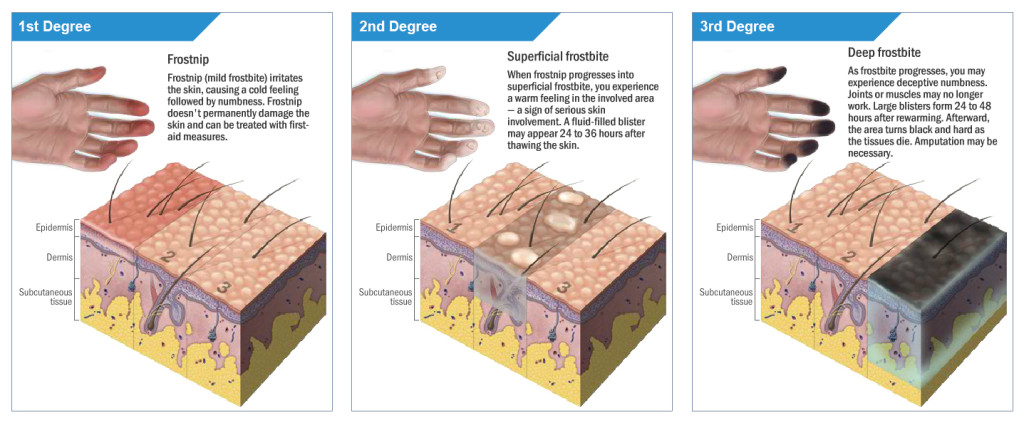
Frostbite generally affects exposed skin and extremities, such as the fingers, toes, nose, cheeks, chin, and ears. Much like burns, frostbite has three levels of severity, known as degrees:
- First Degree (Frostnip) – The outer layer of skin becomes irritated and begins to freeze, leading to a cold feeling and tingling pain. This soon leads to numbness, as well as a red or blotchy discolored appearance. Damage is usually not permanent at this stage.
- Second Degree (Superficial) – Skin will begin to harden as it continues to freeze, but deeper tissue will remain relatively soft. A deceptive sensation of warmth may occur, causing victims to remain unaware of the damage that is occurring. Rewarming at this stage will turn skin blue or purple, and fluid-filled blisters will begin to form within a few days.
- Third Degree (Severe) – Freezing will continue from the surface through the deeper tissue layers. Skin will feel very hard and waxy. The victim may lose all feeling in the area, as well as the use of affected joints or muscles as nerves are destroyed by the cold. Rewarming at this stage will result in large blisters, and the skin will turn black and hard. Surgery and/or amputation may be necessary.
Treatment
If the signs of frostbite are recognized, action should be taken immediately to prevent further damage. As you may have guessed, the key to treating frostbite is warmth. However, care must be taken to control the rewarming process, otherwise more damage can be done.
The following infographic from the Centers for Disease Control and Prevention (CDC) shows the general recommended steps for treatment of frostbite, which also apply to treating a low core temperature (hypothermia):
In more specific terms, here’s the treatment process, as recommended by the Mayo Clinic:
- Get emergency medical help, if at all possible. Immediate treatment by medical professionals is always the best-case-scenario.
- Protect skin from additional cold and exposure. Get to a warmer location ASAP.
- Avoid bending, stretching, or putting pressure on frostbitten skin. DO NOT rub or massage frostbitten skin, it will only cause more damage.

Use ambient temperature or warm water to treat frostbite, rather than direct heat from a fire. - Gently rewarm frostbitten areas by soaking in warm water (99F to 108F). Avoid using direct heat or open flames, as numbness can lead to overheating and burns.
- If water is unavailable, use layers of clothing and body heat. For example, hold your hands under your armpits.
- Don’t allow thawed skin to refreeze. This could make the damage far worse.
- Tingling, burning, and redness will indicate that blood flow is returning. Ibuprofen pain medication can be used to reduce swelling and pain.
Again, these steps are not substitutes for proper medical care. If at all possible, see a doctor immediately if blisters occur, as they indicate second- or third-degree frostbite.
Prevention
It should be clear by now that frostbite is a truly miserable condition, so the best plan is to avoid it altogether. Simple preventative measures can go a long way to stave off frostbite, as well as the hypothermia that often follows:
- Limit Exposure – If you’re outdoors in freezing conditions, frostbite is less a matter of “if” and more a matter of “when”. Take breaks to warm back up, rather than trying to tough out the cold.
- Wear Warm Clothing – Mittens or gloves, moisture-wicking socks, ear muffs, a hat or face covering, and layered undergarments will keep you toasty and dry. Avoid apparel that fits too tightly, as it can restrict blood flow and put you at risk.
- Food and Drinks – Consume warm food and beverages, and be sure to stay hydrated. Avoid alcohol — it may make you feel warm, but it will cause you to lose heat quickly.
- Stay Active – Physical activity will dilate blood vessels and keep your blood flowing. However, be careful not to sweat excessively or exhaust yourself, as this will make the situation worse.
- Watch for Warning Signs – Pay close attention for the warning signs listed above, even if you feel fine. Noticing frostbite early can help you treat it promptly and recover quickly.
For more information on frostbite how it relates to hypothermia, pick up RECOIL OFFGRID Issue 18, on sale January 27th, 2017. In the 411 column titled “Hypothermia Versus Frostbite”, John Schwartze compares and contrasts the warning signs of these two common winter medical conditions.







