In This Article
It’s a deeply rooted fear in the psyche of our culture. What would happen if a large-scale, deadly disease outbreak occurred in close proximity to where we live? Our minds quickly run to scenes from films like Outbreak, Contagion, or I Am Legend as far as how the public would react and what the government would do to intervene.
After we stopped hyperventilating about the possibility of roadblocks being set up, curfews being implemented, and soldiers in hazmat suits herding infected people into quarantine zones, we asked ourselves, “Are these realistic situations, or are we victims of Hollywood lore?” We were curious ourselves about what government protocol is for dealing with outbreaks and went to the experts to find out.
What is an Outbreak?
Actually this term is somewhat subjective and unfortunately gets thrown around, particularly by the media, without proper context. However, there are some terms with which the Centers for Disease Control and Prevention (CDC) describe disease levels, and the term “outbreak” is synonymous with “epidemic.” The CDC doesn’t have epidemic thresholds for every disease, but are always monitoring disease levels throughout the world. These terms defined by the CDC can help shed some light on the amount of pathogens present in a population at any given time.
Endemic: The constant presence and/or usual prevalence of a disease or infectious agent in a population within a geographic area. (For example, Ebola is endemic to West Africa, but not the United States.)
Epidemic: Increase, often sudden, in the number of cases of a disease above what is normally expected in that population in that area.
Outbreak: Same definition as epidemic but is often used for a more limited geographic area.
Pandemic: An epidemic involving several countries or continents, usually affecting a large number of people.
Health Emergency Response

A health emergency in itself is a complex thing with many variables. Although the CDC, the World Health Organization (WHO), and Council of State and Territorial Epidemiologists mandate that when certain pathogens are diagnosed at the local level that they be reported to higher authorities, such as the Ebola discovery in Texas, it doesn’t necessarily mean a public health emergency will be declared or federal involvement is automatically triggered.
A disease outbreak has certain elements that determine the appropriate response. How fatal is the pathogen? What ways is it communicable? How many are believed to be infected? Are vaccines or treatments available to deal with it? These are all factors that determine the best methods for treatment and containment when first identified.
“There is not a single protocol for responding to a public health emergency,” says Jason McDonald, spokesman for the CDC’s Office of Public Health Preparedness and Response. “As you can imagine, a disease outbreak is handled differently from a natural disaster. Even among disease outbreaks, none are handled the same.”
As examples, the recent discovery of E. coli linked to Chipotle restaurants would warrant a different response than the SARS outbreak first reported in Asia in 2003. SARS is an airborne contagion, but E. coli is not transmitted person to person and is usually linked to contaminated food.
Calls to Action
A number of guidelines at the local level, as defined by the Office of Assistant Secretary for Preparedness and Response (ASPR) and the CDC, would be implemented to handle highly infectious diseases like Ebola when they’re initially discovered. Once the infection is reported and confirmed, the state health department would report it to the CDC, which collaborates with WHO. They start monitoring the number of cases recorded through a database of hospital admissions and discharged patients to track the trend. Local agencies ultimately make the determination if more help is needed for treatment and containment based on the number of cases they are seeing.

States have their own public health emergency plans, usually available to view on state health department websites. There are some federal programs built to deal with the consistencies that all emergencies share, but there are also different programs for different purposes.
“There are public health emergencies that do not involve diseases,” says Elleen Kane, who handles strategic communications at U.S. Department of Health and Human Services (HHS). “Most public health emergencies are declared for natural disasters, not diseases. It’s not so much of a hierarchy as it is a collaboration.
“Federal public health emergency response is led by HHS. The ASPR is the primary advisor to the HHS Secretary on matters of bioterrorism and other public health emergencies and, on behalf of the Secretary, ASPR usually coordinates federal resources for emergency response. The National Response Framework (NRF) guides emergency response in general and, in that framework, HHS leads the federal public health and medical response to emergencies.”
In this issue’s What If? article on page 20, we fictionalized some elements of a pneumonic plague outbreak and response for dramatic effect to see how our subject-matter experts would react to those circumstances. However, there are so many variables, it’s impossible, even in the event of a pathogen that serious, to predict the exact level of federal involvement that would take place in real life.
“There are cases of plague that occur every year. They’re noteworthy, but there’s not a federal team that gets called in every time a case is identified,” says Dr. Stephen Redd, director of the Office of Public Health Preparedness and Response. “There might be circumstances where the likelihood of the normal route of exposure was not something that’d be the leading hypothesis, and it might be some intentional exposure release where different groups would come into play, including law enforcement. That would be something where the federal involvement would occur more quickly than a natural case of plague.”
Just so we’re clear on departments, the Federal Emergency Management Agency (FEMA) is an agency within the Department of Homeland Security (DHS). The CDC is an agency within the HHS. All public health and medical support for a state is handled by HHS. Within the HHS, the CDC is typically the lead operational element in disease outbreak situations. Just like the FBI or the DEA, their roles are different, but they all work together when called upon to respond to emergencies and investigations.
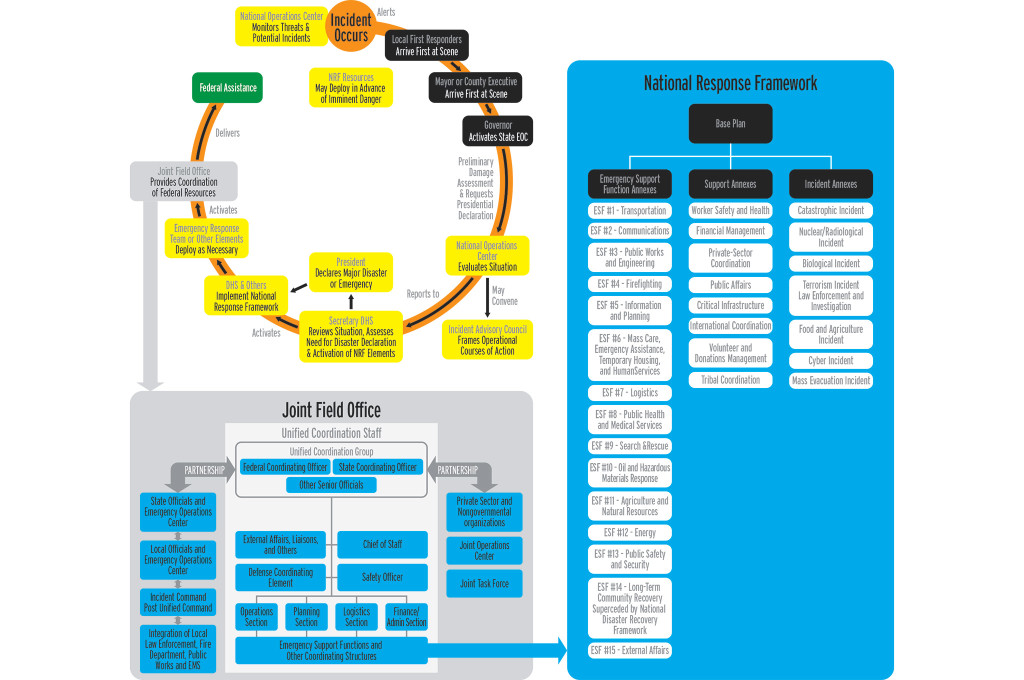
The National Response Framework
Created in 2008, the NRF was developed by the DHS and is managed by FEMA. It builds upon the National Incident Management System (NIMS), which basically serves as a guide to help government and nongovernmental organizations structure their resources to work together to prepare for, respond to, and recover from domestic incidents. It’s written in such a way that it’s always in effect.
NRF uses NIMS to create a framework for coordination among federal, state, local, and nongovernmental organizations, but it’s intended to be used by the whole community. NIMS coordinates the response structure at emergencies, and NRF governs resources used during and after the designated event or incident. The NRF is mandated and applies to all federal departments and agencies that may be requested to provide assistance. It integrates prevention, preparedness, response, and recovery into one comprehensive plan.
Since no threat exists in isolation and often involves collateral damage, the overall goal is to save lives, protect property and the environment, and restore essential services and infrastructure to help communities return to normal.
In an effort to illustrate how this would look on a macro level, we created a graph to illustrate the likely domino effect a major outbreak or public health emergency might trigger as it relates to the National Response Framework.
Public Health Emergencies
A public health emergency (PHE) can be declared in preparation for, or in response to, a potential public health crisis to deliver necessary resources. This was done in 2009 for the flu pandemic and could include anything from a natural disaster to a bioterrorist attack — or anything else the president or HSS secretary believe represents a threat to public health. It lasts for 90 days and can be renewed or terminated early if deemed necessary.
The president or HHS secretary can make the declaration independent of each other, but the president may only do so under the Stafford Act, which authorizes financial assistance for the response or mitigation efforts. Presidential disaster or emergency declarations are separate and distinct actions that don’t have the same conditions as a public health emergency. Unlike disaster or emergency declarations that typically require the request of a governor (if he or she feels the magnitude of the emergency goes beyond the state’s capability to handle it), a public health emergency can be activated without a governor’s request. A presidential declaration may be required to grant the HHS secretary certain authorities.
Quarantines
If you travel, especially internationally, you’ve probably seen literature distributed about pathogens to be aware of while at your destination or wherever you may be returning from. Monitoring ports of entry is vital to defend against the introduction of potential health threats into our communities.
A quarantinable diseases list is contained in a presidential executive order. It’s amended periodically, but it grants officials federal quarantine and isolation authority to apprehend, examine, or conditionally release someone who’s known or believed to be infected with a disease on the list. States are responsible for controlling the spread of a disease within their borders. Their laws vary on the topic, but can also authorize the detainment of individuals to prevent the spread of disease.
As there are differences between the two, it’s important to differentiate isolation from quarantine:
- Isolation is the practice of separating and restricting movement of ill persons found to be infected with a quarantinable disease. This is standard procedure in hospitals with diseases such as tuberculosis.
- Quarantining is the separation or movement restriction of a well person believed to have been exposed to, or possibly carrying, a quarantinable disease in its communicable or pre-communicable stages.
At ports of entry in particular, the CDC serves the primary role for implementing measures to control the spread of diseases. Public health authorities at the state, local, or federal level may request assistance from law enforcement to impose a public health order. The U.S. Customs and Border Protection (CBP) and Coast Guard are required, under the Public Service Health Act, to assist the CDC in enforcing quarantine regulations. The CDC, or agencies required to assist in enforcing their regulations, may detain the travel of someone thought to be ill for purposes of examining the cause of their illness and whether it’s communicable.
Military Intervention
National Guard members have expertise in critical areas, such as emergency medical response, nuclear response and planning, and decontamination. The NRF states: “The governor may activate elements of the National Guard to support state domestic civil support functions and activities. The state adjutant general may assign members of the Guard to assist with state, regional, and federal civil support plans.”
In other words, if the situation calls for it, the military can and will be used to protect human life. This doesn’t necessarily mean martial law or things seen in movies will automatically be activated. For instance, as we talked about domino effects disasters tend to create, the National Guard, Coast Guard, CBP, and various other auxiliary organizations were all called upon to assist in different tasks during the aftermath of Hurricane Katrina and support local law enforcement. Although there isn’t an official threshold for military involvement, it may be deemed necessary.
Planning and Reliable Information
If you start hearing gossip of an outbreak on the news, you should also turn to the experts to gather more info and precautionary advice than what you may first be hearing. “Although it’s thought of as an enhancement of our ways to communicate, the Internet and social media can be very detrimental in these circumstances,” says Dr. Robert Quigley, senior vice president of medical assistance for International SOS. “In a matter of seconds, information can be disseminated and a lot of it can be fictional and not factual, and that doesn’t help us.”
The government will use whatever means they can to disseminate news regarding public health threats, but one should also confirm what they are hearing through conventional outlets to ensure it’s legit. Websites such as www.phe.gov and www.cdc.gov provide reliable, substantiated information.
The HHS and the CDC have other resources to educate yourself on health concerns as well. Training and education centers for Ebola and other disease have been set up and the CDC’s Journal of Emerging Infectious Diseases is a free monthly publication that anyone can sign up for (wwwnc.cdc.gov/eid/subscriptions). Clinician Outreach and Communication Activity calls and webinars are also available to participate in through the CDC website.
Awareness and Prevention
“The virus that has the potential to be highly transmissible and has a high degree of severity is pandemic influenza,” Redd says. “That would be an influenza that is transmissible the way seasonal influenza is, but has a different genetic structure, so we don’t have an immunity to it. If that causes a severe disease that’s slowly transmissible, that would be a big problem.
“That’s basically what the H1N1 pandemic was — a virus that hadn’t been seen in people before that was readily transmissible. Fortunately that virus didn’t have a high hospitalization or mortality rate, but a different virus could be much more severe.”
As mentioned in the article “Condition Red” in our Winter 2015 Issue, there are common-sense hygienic practices people should engage in if they’re traveling. If you’re home and an outbreak is reported, visit the previously mentioned information sources, be conscientious of your own health, and take care not to spread something if you’re sick or become infected. Wash your hands often, stay home if you’re sick, get any available vaccinations before you become ill, and seek medical attention if you feel sick, particularly if its symptoms are consistent with any illnesses reported in public health alerts.
You may also want to double down on receiving health alerts and advice by aligning yourself with an assistance company such as International SOS, which provides up-to-date notifications and support to travelers and businesses domestically and internationally.
The first line of defense begins with the public and their willingness to stay informed and responsible.
“Because of ease of travel and globalization of our workforce, we’re always going to be at risk of someone introducing an infectious disease from an area where it’s endemic,” Quigley says. “It’s another reason why companies should have pandemic plans, business continuity plans, best practices of infectious disease controls in place, and if they’ve done all of the above, the likelihood of infectious diseases coming into our community and spreading into anything more than a minimal outbreak will be limited.”
Health security starts with you.
Federal and International Plans
You can check out these plans created by the following organizations in their entirety by visiting these links.
FEMA
- National Response Framework
- www.fema.gov/media-library-data/20130726-1914-25045-1246/final_national_response_framework_20130501.pdf
- National Response Framework (annexes supplement)
- www.fema.gov/pdf/emergency/nrf/nrf-annexes-all.pdf
ASPR
- National Health Security Strategy and Implementation Plan
- www.phe.gov/Preparedness/planning/authority/nhss/Documents/nhss-ip.pdf
CDC
- Public Health Preparedness Capabilities
- www.cdc.gov/phpr/capabilities/dslr_capabilities_july.pdf
- All Hazards Preparedness Guide
- www.cdc.gov/phpr/documents/ahpg_final_march_2013.pdf
WHO
- Emergency Response Framework
- www.who.int/hac/about/erf_.pdf
- Global Influeza Preparedness Plan
- www.who.int/csr/resources/publications/influenza/WHO_CDS_CSR_GIP_2005_5.pdf
More From Issue 12
Don’t miss essential survival insights—sign up for Recoil Offgrid’s free newsletter today.
- A Bug Out Toyota Tacoma Fit For A U.S. Marine
- Insulated Gloves & Mittens Guide – [N]ICE And Warm
- Government Response to Disease Outbreaks – Outbreaking News
- What If An Outbreak of Weaponized Pneumonic Plague Hits Your City?
- Hydroponic Growing Systems – Hydro Planting
- How to Strengthen Your Defenses – The Master Key
- Lights Out: Chokehold Basics for Self-Defense
- Biggest Outbreaks in U.S. History
- Human Lie Detector
- Learn How To Start Fires In Cold Weather
- Disposable Vs. Rechargeable Batteries – In Charge
- How to Survive a Structural Collapse
- High-Lumen Flashlights
Read articles from the next issue of Recoil Offgrid: Issue 13
Read articles from the previous issue of Recoil Offgrid: Issue 11
Editor’s Note: This article has been modified from its original print version for the web.