In This Article
Did you ever think that Sigmund Freud would be found in the pages of RECOIL OFFGRID? Freud is often cited as the originator of the pleasure/pain principle. This principle suggests that we’re born into pleasure and avoid pain at all costs. The problem is that we don’t always have control over pain. And when it comes to pain management, there can be all kinds of shades of gray as to how it feels and how we respond to it. Our mindset is probably the most important factor in dealing with both acute and chronic pain. Tools, such as medication, are also helpful in easing pain.
The Psychology of Pain
Everyone handles pain differently. Pain management has both a physical component and an emotional component. Physical pain can be different from one individual to the next because of our different genetic makeups. The emotional component also varies based on past experiences associated with pain. The patient’s perspective of their experience is different than my perception of their pain. This is what makes treatment of pain difficult as a physician.
I think that understanding the patient and their past experiences is the key to understanding how they handle pain. Some people will be tough as nails and work through pain and injury to complete their mission. Others will crumple on simple tasks, because they don’t mentally handle their pain well. About half of the treatment of pain is listening and understanding the patient’s perception of what the pain is and how it debilitates them. The other half of treatment is creating a plan that gives the person hope for a better tomorrow.

Above: Even those who exercise regularly and eat well can often experience sudden pain. Don’t be cavalier about it. Over-exerting yourself with the assumption that it will “just go away” may make a bad situation worse.
In order to work through pain, it takes some mental fortitude on the patient’s part and some words of encouragement from everyone else. Understand that there’s a diference between pain and injury. Pain is something you can mentally work through and overcome temporarily to complete your mission. Focus on anything besides what’s causing the pain, and you’ll succeed. Take one step at a time. Sing one song at a time. Pick a landmark ahead and focus on reaching that goal. Pain will want to draw you back to giving in to it, but fight on. However, an injury may need to be addressed before continuing on with the mission. Maybe you lacerated your leg on a rock, and it needs attention. Maybe you fell and broke a bone. Perhaps you need to fashion a splint (check out Dr. Joe Alton’s article “Medical Improvisations” in Issue 36 of RECOIL OFFGRID). Treat the injury to the best of your ability.
Inflammation
We almost all recognize inflammatory pain. That throbbing, aching sensation that limits mobility, especially in a joint, can happen in any scenario. When an injury occurs to tissue, the body increases blood flow to the area. The blood carries cells from your immune system to help repair any damage. The area of concern becomes red and warm to touch due to the increased blood flow. Along with the blood comes increased swelling, from the by-product of what the inflammatory mediators are doing to the affected tissue. The pain comes not only from the injury and damaged tissue, but also from the swelling within the tissue. This is your body’s way of trying to keep you from further injury by making you limit your activity.
You may be familiar with the RICE mnemonic that was introduced by Dr. Gabe Mirkin in 1978. It has long been a standard procedure for acute musculoskeletal injuries. Rest, Ice, Compression, and Elevation were thought to be important in the first 24 to 48 hours of injury. The idea behind rest was to prevent further injury. Ice, compression, and elevation were to be used to decrease the amount of swelling in the injured area. Recently, there have been arguments against this model, including from Mirkin himself. He has suggested that rest and ice may not be the best after all and that this treatment slows healing. He now advocates for movement, and no ice, for the acute injury. Just stick to compression to limit swelling and elevation to help the blood flow return to the heart.
When should an anti-inflammatory medication such as ibuprofen or naproxen be used? Well, that depends. If you want the damaged tissue to repair itself in a natural fashion, then don’t use an anti-inflammatory. The tissue will take time to heal, though, and you may not be able to afford that time in a bug-out situation. If, on the other hand, you need to move through the pain, you could take the medications as needed. Anti-inflammatories work well with acute pain. When there’s no pill to take, you could forage for wild onion or garlic. These have anti-inflammatory properties and also boost your immune system. You might be lucky to find a willow tree. The inner bark contains salicylate-like properties, which will act like aspirin. The downside is that these options won’t be as potent as ibuprofen, but they may provide some relief that allows you to get back to safety.
Neuralgia
When pain comes from the nerve, it’s called neuralgia. Neuropathic pain can be elicited centrally or peripherally. When peripheral pain occurs, it can be due to lack of blood supply to the nerve (e.g., advanced diabetes) or metabolic deficiencies (e.g., vitamin B12 deficiency or thyroid hormone deficiency). This usually occurs in a fairly chronic setting and isn’t an acute event. It can feel like a numb sensation or no sensation at all. It may also feel like a tingling sensation. When the pain comes from a central location, it can be something pressing on a nerve near the spinal cord (e.g. tumor or intervertebral disc) or something that severed the nerve (e.g. trauma). The pain can be mild and consist of a pins-and-needles sensation, or it can be severe like an electric shock or burn that doesn’t go away. This can be seen in both an acute setting as well as chronic, as in a bulging intervertebral disc.

Above: Above: Pain can be influenced by any number of factors, including age, activity level, pre-existing injuries, and heredity, just to name a few. If the onset of pain doesn’t improve with rest or is accompanied by other problems, seek immediate medical attention.
In a survival situation, the more common causes of neuralgia are from trauma. If you inadvertently cut yourself with an edged weapon (acute peripheral neuralgia) or fall from an elevated position and injure your back (acute central neuralgia), the solution to improve your situation isn’t easy. In the event of a severed nerve, you first need to stop the bleeding associated with the injury. The nerve will likely retract, and if there’s no immediate attention, there could be permanent damage and loss of function. Depending on which nerve is cut and what muscle it’s associated with, movement to safety may be a challenge. If your back is injured to the point where a disc between the vertebrae has been “slipped” or even herniated, the fix isn’t a quick one either. This too could affect mobility and, ultimately, your safety in a survival setting. Keep in mind that with the trauma you’ll also likely have musculoskeletal injury, which will hinder movement.
In a hospital setting, with a back injury, a combination of muscle relaxers, narcotics, and steroids (or anti-inflammatories) would be ideal. In this case, an anti-inflammatory would be needed due to the severity of inflammation and lack of mobility. The muscle relaxers would help with mobility by lessening the pain of muscle spasms. The narcotics are great for severe and acute pain management, but should not be used for chronic conditions. People tend to build a tolerance to narcotics, so the longer they’re used, the less effective they become. Some people are so afraid of their chronic pain that they depend on their narcotics as a crutch rather than face their fears associated with the pain. This situation has contributed to the “opioid crisis.”
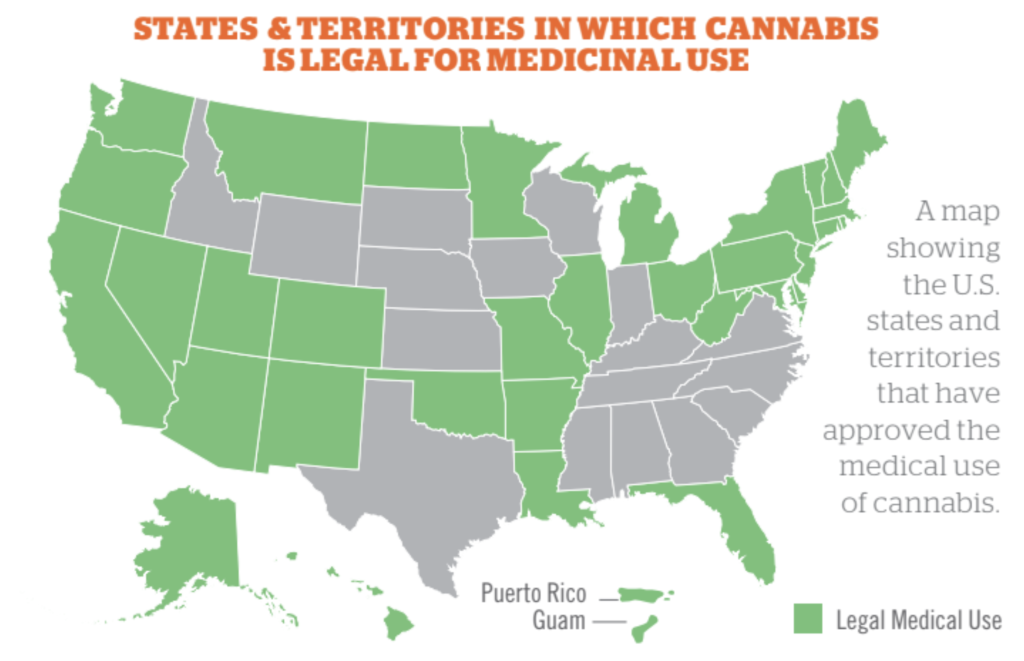
Marijuana’s Role in Pain Management
The “wacky tobacky,” as my uncle used to call it, has been used for thousands of years for its medicinal properties. The popularity in the past few years in the U.S. has likely centered on revenue more than around healing potential. However, I’ve had many patients try it for chronic pain with good success. I don’t believe that it has been shown to help with acute pain.

Above: Various glass bottles with CBD oil, THC tincture and hemp leaves on a marble background. Copy space, mockup. Cosmetics CBD oil
Although there’s ongoing research on the use of marijuana for pain relief, there isn’t much known about why it works. The endocannabinoid system (ECS) is something in our body that naturally produces some amounts of cannabinoids. The ECS seems to be involved in helping with pain management, inflammation, appetite, anxiety, sleep, mood, and many more aspects of our body’s homeostatic mechanisms. Whether our body produces it naturally, or we consume it in the form of THC (tetrahydrocannabinol) or CBD (cannabidiol), we have two known receptors in our body where it has its effect. The CB1 receptor is generally associated with the central nervous system and helps with pain. The CB2 receptor is generally associated with the peripheral nervous system and helps with inflammation. Understand that these are huge generalizations and that each receptor likely has other roles as well.
In my professional experience, THC has been extremely helpful in people with chronic pain management and cancer. I’ve seen people reduce the amount of narcotics they consume once they switch to marijuana. I’ve also recommended it for patients with cancer who’ve lost their appetite. It has been really good at boosting their appetite to get them through their chemotherapy treatments. The downside of lighting up is the possibility of a fast heart rate (tachycardia), anxiety, paranoia, and cyclic vomiting syndrome. Many states now have medical marijuana dispensaries that are controlled by the government and filled with red tape.
CBD, usually in oil form, works a little differently than THC, and its mechanism of action isn’t completely understood. I’ve seen people use this with great success on chronic inflammation. It doesn’t work with acute pain management at all, in my professional experience. The downside of using CBD oil is its expense and the amount of time it takes to start working, often weeks.
In Summary
Pain is a poorly understood phenomenon. Understanding the difference between pain and injury can get you through a difficult and traumatic situation. Knowing basic medical treatments can be helpful in stabilizing the injury. To treat pain properly, it helps to know what type of pain source you’re facing. The medications can then be directed accordingly. Keep in mind, in an austere setting, you may need to be creative with your treatments. The more you know about herbal medicine, the better prepared you’ll be to offer assistance. Remember that pain management is also a mental challenge, especially in a remote location. Stay positive and break things down to manageable tasks. If you have chronic pain, the challenge is overcoming the demons that prevent you from moving forward. An acute injury on top of chronic pain can seem impossible to overcome, but you can do it. Take baby steps and keep moving!
Further Education:
- No Excuses: Train through the Pain.
About the Author:
David L. Miller, DO, FACOI, is an internist in private practice for 20 years. His experiences away from the office have included time as a fight doctor in regional MMA events and as a team physician for 10 years at a mid-major university in the Midwest. Currently, he serves as the lead medical instructor for the Civilian Crisis Response team based out of Indianapolis.
WARNING:
This article is meant to be a general overview and is not a replacement for medical advice or training. Consult with your doctor before attempting any of the techniques described here.

