In This Article
Disclaimer
This article is meant to be a quick overview and not a detailed guide on how to deal with diabetes in an emergency situation. Professional medical treatment should always be sought first before attempting any of these methods.
Surviving an apocalyptic event will be a serious challenge for healthy people. As both a doctor and a Type 1 diabetic, I can say that the challenge is more formidable for those of us with this chronic condition. Preparation is necessary to survive for any amount of time, especially for a diabetic.
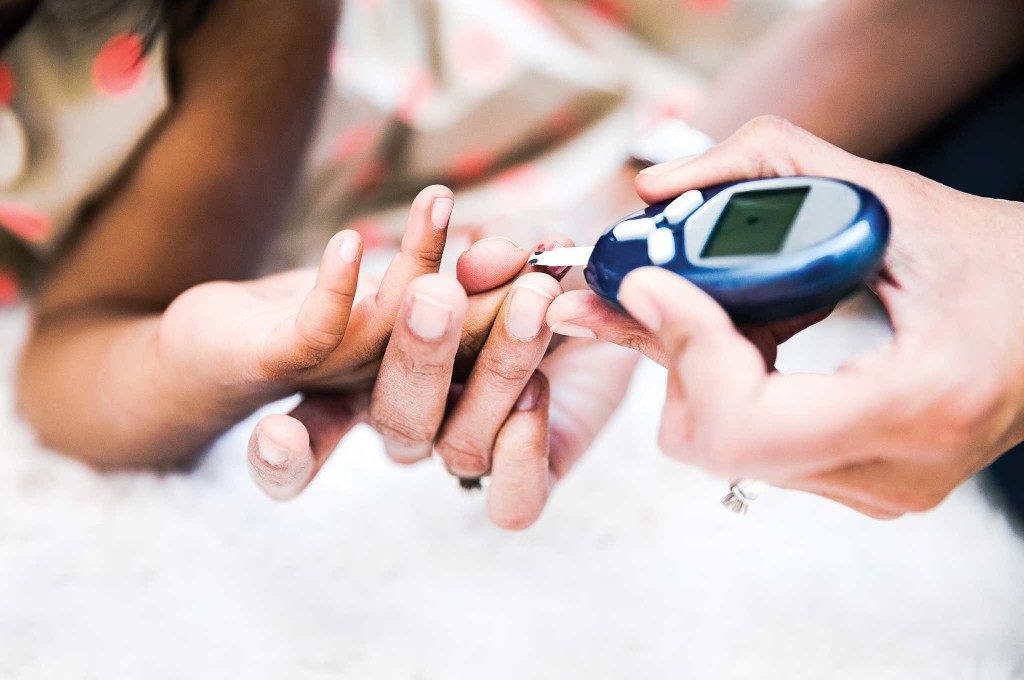
Diabetes is a1 disease of the balance between calories consumed and insulin produced (or injected). Normally, a diabetic should aim for a blood sugar of 110 to 130; however, in a survival situation I would recommend a blood sugar near 180 to 200. Your body is much more tolerant of high blood sugars (hyperglycemia) in short-term survival situations; low blood sugars (hypoglycemia) can quickly be deadly below 20. Taking the time to prepare and acquire the diabetic supplies you need could mean the difference between life and death.
Important Supplies
In the event of an emergency you may not have time to get your gear and enough medications together quickly. Most of us will have a bug-out bag and extra basic supplies to give ourselves a chance to last for a while. However, as a diabetic, you’ll need time to acquire all the supplies you’ll need to last days, weeks, or possibly months. Supplies to consider include medication, syringes for insulin, test strips, two glucometers, a solar charger, batteries, glucose, and water purification equipment.
With different medications, there are important factors to consider. Every medication has a shelf life and expiration date. As a general rule, for prescription medications in pill form, I will keep them up to one year after I acquire them; after one year, I dispose of them. Keep them somewhere cool and away from direct sunlight. Insulin is best kept in the refrigerator, but it may be kept at room temperature for up to a month without losing its potency. The warmer the temperature, though, the faster the insulin will become ineffective. If the insulin is past the expiration date or has been sitting at room temperature for 30 days, I wouldn’t recommend using it.
Metformin is a popular pill for diabetes, but if you are dehydrated and your kidney function declines, this drug can cause lactic acid to build up in your system. Your chance of dying due to lactic acidosis is twice as high if this happens so make sure you stay hydrated! Glipizide and Glimepiride are two other medications commonly used for diabetes. These two medications are usually tolerated well even when your body is under stress.
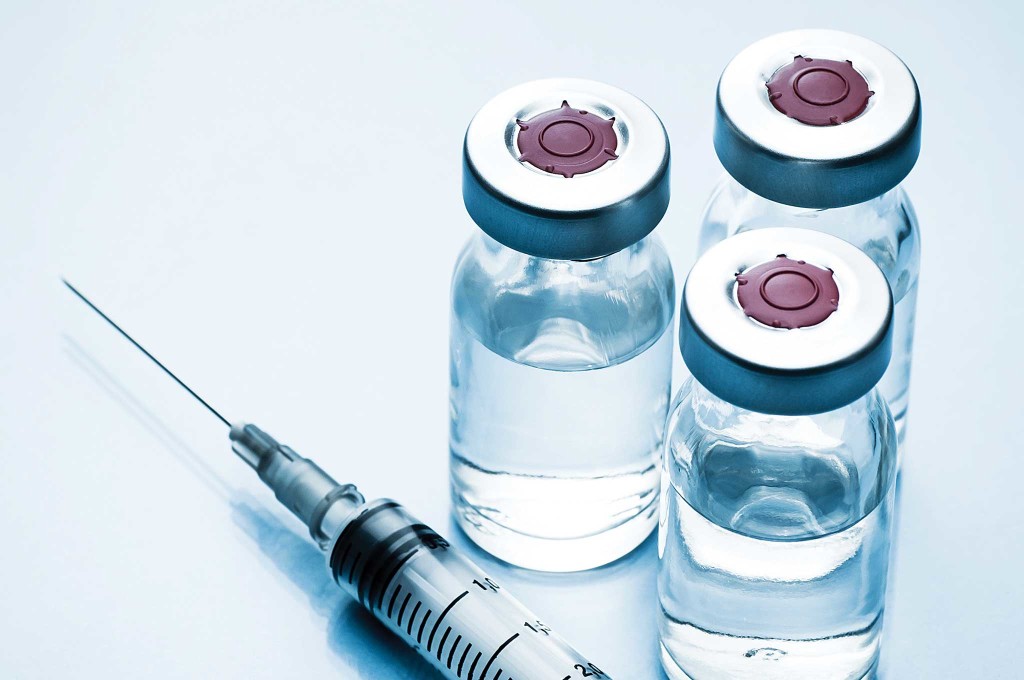
There are many types of insulin (e.g., long acting and combinations of long and short acting). They come in 10mL vials or 3mL pens. Knowing what your type of insulin will do for you is incredibly important before an emergency. If you don’t know, ask your doctor. Keep in mind that insulin can be kept at room temperature for about 30 days if needed. Make sure you have enough syringes or pen needles for four injections a day. I don’t recommend reusing these.
For testing blood sugars, you should have two of the same meters and enough strips to test four times a day. Keep a few batteries as backup. Some meters now come with USB chargers and no separate batteries; thus, it is a good idea to have a solar charger.
If you’re an insulin pump user, a solar charger can also be used to charge your pump. Having enough supplies for your pump is important, but will take up a lot of room. Most pumps now have continuous glucose monitoring capabilities and are an excellent way to monitor your sugars in a survival situation. The most important thing for pump users, however, is to be comfortable going back to injections in the event your pump quits working or you run out of supplies.
Proper Preparation
If a disaster were to occur today, would you have all of the diabetic supplies you needed to survive for any amount of time? You should anticipate needing three months of supplies in the worst-case scenario. After those three months, you may be able to scavenge supplies from casualties. In order to save enough supplies, you may need to prepare a year in advance of a SHTF scenario. Since it is impossible to predict when that event will occur, you will need to have a plan in place to improve your odds of survival.
When you think about stockpiling medication, realize that most insurance companies will allow you to pick up your prescriptions five days early. If you are taking oral medication once a day, filling it five days early will allow you to collect five extra days of medications a month. With insulin, the amount you need will depend on how much you use and whether you use long-acting or short-acting insulin. In general, the older insulins are U 100, which means that there are 100 units of insulin per 1 mL. Vials of insulin have 1,000 units (10 mL) and pens have 300 units (3mL). Newer insulins are concentrated (U 200, U 300, and U 500) and have more insulin per milliliter. As an example, if you take 30 units a day of U 100 insulin then you will use 900 units a month. That leaves 100 units extra each month. If you still pick up your prescription on time every month then in 10 months you will have stockpiled one vial of insulin. Insulin pump users should stockpile pump supplies, but also have backup syringes in the event the pump fails.
For test strips, keep in mind you will probably need to be checking your blood sugar more frequently the longer the survival situation persists. Be sure you refill your tests strips monthly even if you don’t use all the allotted strips. By doing this, you may be able to procure several hundred extra strips within a year. When you find that you have to check your blood sugar four times a day in a survival situation, these surplus strips can last months.
Make sure you are keeping the test strips in a dry, cool place to help them last longer. I wouldn’t recommend using test strips beyond the expiration date due to the potential for less accurate readings. Usually your meter will come with a control solution which tests your meter’s accuracy. Most meter companies will send you a control solution for free if you call the number on the back of the meter. Ask your doctor about getting a spare meter or call the meter company: they often have extras to give to you.
What to Expect
The stress of a survival situation will likely increase your blood sugars in the first few days. The stockpile of medications will help with hyperglycemia, and the food storage (e.g. canned goods and MREs) you have saved should help combat the hypoglycemic events early on. You should be checking your blood sugars one to two times a day at this point.
As the event moves from days to weeks, checking your blood sugar is more important (two to three times a day). Your food sources will begin to dry up, and you’ll now need to forage for food and water. The risk of hypoglycemia increases as your energy expenditure increases and caloric intake decreases. I would recommend checking at least four times a day as the disaster stretches from weeks into months.

The possibility of death due to hypoglycemia increases the longer the survival scenario persists. The ability to be productive when the blood sugar drops below 60 is difficult, and the ability to survive once it drops into the 20s isn’t guaranteed. Resources such as glucose tablets, glucose gel, and glucagon pens are an option to fight hypoglycemia, but aren’t long-term solutions. Knowing what kinds of fruits (e.g. raspberries, blackberries, oranges) grow naturally in your area will also be helpful if your sugar goes low. High-calorie emergency ration bars can contain 400 calories per bar and may be used as a bridge until food can be procured. These items should also be stockpiled.
In Summary
As a diabetic, the importance of stockpiling medication and resources for a survival scenario cannot be overemphasized. It’s important to know how your body and blood sugars respond to stress. Maintain a balance during a crisis situation, and you’ll be better prepared to succeed.
About the Author
David Miller, DO, FACOI, is an internist in private practice. Diagnosed with Type 1 diabetes in 1990, he has a unique perspective on patient care and disease management. Experiences away from the office have included being a fight doctor for regional MMA bouts and a team physician for a Division I university in west central Illinois. Dr. Miller is an instructor for the Civilian Crisis Response Team (medical section) based out of Indianapolis.
More From Issue 24
Don’t miss essential survival insights—sign up for Recoil Offgrid’s free newsletter today!
- Carrying & Dragging Techniques – Let’s Get Carried Away
- Multi-Tools Buyer’s Guide
- Issue 24 Gear Up
- Review: Dometic CFX35W Portable Refrigerator Freezer
- Review of Prepper Guns by Bryce M. Towsley
- The Myths of Dealing With Frostbite
- Merino Wool Baselayers Buyer’s Guide
- The Diabetic Survivalist
- Advanced Fire-Starting Techniques in Cold Weather
- What If Your Cruise Ship Is Hijacked?
- Hiking Boot Buyer’s Guide – Take a Hike
- Lost In The Wild Survival Tips – Get Lost
- How E.J. Snyder Paved a Road to Survivalist Success
- Must-Have Items for Survival in Hostile Regions
Read articles from the next issue of Recoil Offgrid: Issue 25
Read articles from the previous issue of Recoil Offgrid: Issue 23
Check out our other publications on the web: Recoil | Gun Digest | Blade | RecoilTV | RECOILtv (YouTube)
Editor’s Note: This article has been modified from its original version for the web.