In This Article
The hero in our apocalyptic thriller has survived the outbreak and taken up residence in an abandoned hunting shack. Soon, that antique radio will be dusted off, and efforts will be made to reach out to other survivors — if there are any. In the meantime, there’s a pristine stream nearby and lots of wild game roaming the woods. Our hero just has to redevelop those hunting and survival instincts that were sacrificed in favor of a more urbane skill set. But what if the mysterious pathogen at the root of it all didn’t just show up at the airport? What if it isn’t coming from zombies or aliens or terrorists? What if it’s carried by the deer, elk, rabbits, and squirrels, and it lurks in rodent nests in the cabin or in the stream outside? This brings us to the topic of zoonotic diseases.
Above: Deer are known carriers of chronic wasting disease (CWD). Like mad cow disease, it cannot be destroyed by temperature during cooking. Contaminated meat requires specialized disposal.
What Are Zoonotic Diseases?
Zoonotic diseases are those that aren’t species-specific but can be passed from animals to humans (or vice versa). No, there aren’t any zoonotic diseases on the horizon that are expected to end civilization, but some can cause serious illness or even death and have left a dark shadow on the history of the world. Hunters, trappers, and farmers have sufficient opportunity to be exposed to these illnesses, but so does anyone who may find themselves cleaning out a storage shed or buying milk or meat from neighbors.
Rabies
Rabies is the first example in any discussion about zoonotic diseases. It’s one that we first heard mentioned in movies and TV shows when we were kids, and while few of us know someone who’s contracted this deadly disease, it’s a big deal globally.
An estimated 24,000 people die each year in Africa from rabies. Asia sees about 32,000 deaths annually, and worldwide, 99 percent of human cases are transmitted by domestic dogs.
It’s a different picture in the U.S., where there were only 23 human cases from 2008 to 2017, and thanks in part to aggressive pet vaccination campaigns, only 65 dogs and 250 cats test positive for the rabies virus in any given year, according to the Centers for Disease Control & Prevention.
Wild animals are the primary carriers of this zoonotic disease. Rabies may be endemic in your region in skunks, bats, raccoons, or foxes, depending on your location. In the East, for instance, the U.S. Department of Agriculture’s Animal and Plant Health Inspection Service (APHIS) is undergoing a program to halt the western expansion of raccoon rabies by dropping vaccine packets from aircraft.
The rabies virus can be transmitted to humans, pets, and livestock via an infected animal’s saliva, normally through a bite, but it’s also possible to contract the virus through mucous membranes. Flu-like symptoms will appear first in a human host, possibly accompanied by itching at the site of the bite. This will quickly progress to anxiety, confusion, agitation, and delirium. Symptoms may show up one to three months after exposure, although incubation periods of up to nine years have been documented. In some cases, so much time has passed from the transmission to the symptoms that victims don’t even recall the wildlife encounter.
Rabies can be successfully treated with one dose of immune globulin and four doses of rabies vaccine over a two-week period if action is taken immediately. Unfortunately, once symptoms begin, death is practically imminent, so it’s important to report any encounters with potentially rabid animals to a physician as soon as possible.
Testing for rabies in animals requires tissue from the brain stem and cerebellum. Therefore, the animal must be euthanized. In humans, testing can be performed with a combination of saliva, serum, spinal fluid, and skin biopsy specimens. However, preemptive treatment is wise if exposure to the virus is likely.
Above: Nocturnal animals that appear listless and disoriented, especially if seen during the daytime, may be infected with rabies.
Hantavirus
In 2004, a graduate student became ill shortly after collecting wild rodent data in West Virginia. It’s believed that sometime during the course of that fieldwork, he inhaled dust stirred by the disturbance of a rodent nest. He died three days after his symptoms appeared. The cause: hantavirus.
People can become infected with hantavirus through exposure to rodent feces, urine, or saliva. In the U.S., it may lead to Hantavirus Pulmonary Syndrome (HPS), a severe respiratory infection, with such early symptoms as fever, fatigue, muscle aches, nausea, vomiting, diarrhea, and stomach pain, from one to eight weeks after exposure to the virus.
No vaccine, treatment, or cure for hantavirus currently exists, but those who are diagnosed early enough can be given an oxygen treatment in an intensive care unit to help their respiratory systems deal with the infection. The Centers for Disease Control and Prevention reports a 38-percent mortality rate for HPS.
Above: Gloves, masks, and a bleach solution are good defenses against hantavirus.
People are at risk of exposure to hantavirus whenever they’re cleaning up areas where mice and rats have been, like cabins, barns, or storage sheds.
Director of the University of Maine’s Veterinary Diagnostic Laboratory, Dr. Anne Lichtenwalner advises the use of a dust mask in those types of spaces. She further recommends opening a door and letting those structures air out for a half hour before going in, then spraying things down with a bleach solution.
“The CDC is developing better recommendations for people who clean up heavy rodent infestations,” she says, “with the primary idea to reduce the tendency to stir up the dust, since that increases the chance of inhaling the virus before sunlight or disinfectants can inactivate it.”
Chronic Wasting Disease
Two things make chronic wasting disease (CWD) unique in our list:
- It’s caused by a neither a bacteria, nor a virus.
- It doesn’t fit the definition for zoonotic diseases, at least not at the moment.
The causal agent in CWD is a prion — a type of protein that causes normal proteins in the brain to fold abnormally. Just like with another well-known prion disease, bovine spongiform encephalopathy (“mad cow disease”) and mad cow’s human version, Variant Creutzfeldt-Jakob Disease, those folded proteins result in rapidly progressive symptoms such as drastic weight loss, stumbling, listlessness, and nervousness. The disease always leads to death.
CWD is highly contagious among deer, elk, and moose, but at this point, there’s no evidence that it can be passed to humans.
Dr. Bryan Richards, Emerging Disease Coordinator with the U.S. Geological Survey’s National Wildlife Health Center in Madison, Wisconsin, explains that much laboratory work and computer models have looked at variables that could move CWD from animals to humans. Some of those models have been successful, but others have not.
“At the end of the day,” he says, “one would have to conclude that the species barrier is robust, but the chance of a human being infected isn’t zero.”
He adds, “And individual risk may change over time as the zoonotic disease passes from deer to deer to deer. After a time, it will reach a stable state, where it’s more likely to pass to an alternate host.”
Hunters and consumers of venison are the most likely candidates to come into direct contact with the prion, and the CDC lists a number of safeguards to lessen exposure. First and foremost, hunters should avoid harvesting deer or elk that appear sickly or are acting strangely. Wear latex or rubber gloves while field dressing or processing the animal. Minimize the handling of organs, especially the brain and spinal cord. Consider having a harvested deer or elk tested through the state’s wildlife management agency, especially if taken from an area with a known disease occurrence. Of course, if the animal tests positive for CWD, don’t eat the meat.
Richards points out that disposal of the carcass after processing can be an issue in and of itself, especially for those who process their own. Many landfills won’t accept deer and elk remains, but to put them back into the environment would open a door for further exposure. So, it’s advised that hunters check with their state’s department of natural resources on the best practices for disposing of carcasses.
Brucellosis
Debates about the legality of raw milk are common in self-reliant circles, and a word that eventually gets brought up is brucellosis. Brucellosis is a bacterial infection marked by night sweats, fatigue, anorexia, headaches, joint pain, and fever. (Human brucellosis is sometimes called undulant fever, because the intensity of the fever rises and falls.) These symptoms appear after an average incubation period of 7 to 21 days, although that’s highly variable and can be as long as several months.
The zoonotic disease is relatively rare in humans in the United States. On average, there were just over 100 cases of human brucellosis reported annually from 1993 through 2010, according to the CDC.
Dr. Terry Conger, a veterinary medical officer with USDA APHIS Veterinary Services in Little Rock, Arkansas, explains that there are three species of the pathogen infectious to humans: Brucella melitensis (normally found in goats and sheep), B. suis (pigs and reindeer), and B. abortus (cattle, elk and bison). The greatest number of human infections in the past several years have been due to B. melitensis.
“Greater than 95 percent of the human cases in the U.S. have been due to the consumption of unpasteurized goat cheese imported or brought in from Mexico,” says Conger. “The other 5 percent of the cases have been due to people travelling to Mexico or other countries where B. melitensis is endemic, where they are exposed to infected goats or sheep or consume unpasteurized dairy products, and coming back to the U.S. with the disease.”
Wild hog hunters are also at risk of exposure. The bacteria can be transmitted through fluid splashing into the eyes during butchering or by eating undercooked meat.
According to the CDC, once a physician confirms Brucella in blood, bone marrow, or other bodily fluids, antibiotics can be prescribed. Only 2 percent of human cases prove fatal.
Tularemia
During outbreaks of tularemia, also known as rabbit fever, rabbits, hares, and rodents may die in large numbers in an area. Tularemia is highly infectious, and anyone who comes into direct contact with rabbits or rodents has the risk of being exposed to the bacteria. Beyond direct contact, it can be spread via tick, mosquito, or deer fly bites. Furthermore, if hay equipment or mowers contact an infected carcass, the pathogen can become airborne and has the potential for infection via inhalation.
Above: When cleaning game, white spots on the liver or spleen of infected animals is one obvious indicator of tularemia.
According to the Center for Food Security and Public Health at Iowa State University, there are six forms of tularemia in humans, many of which manifest flu-like symptoms, swollen lymph glands, or skin lesions. Of the six forms, typhoidal tularemia is considered the most severe and can often lead to pneumonia.
The incubation period for tularemia can range from three days to two weeks, according to the Centers for Disease Control and Prevention. The disease can be treated effectively with antibiotics, but preventing infection is the best defense. Use insect repellents appropriately to avoid bites by vectors. Avoid touching dead animals, or wear gloves when processing small game, and cook wild game thoroughly.
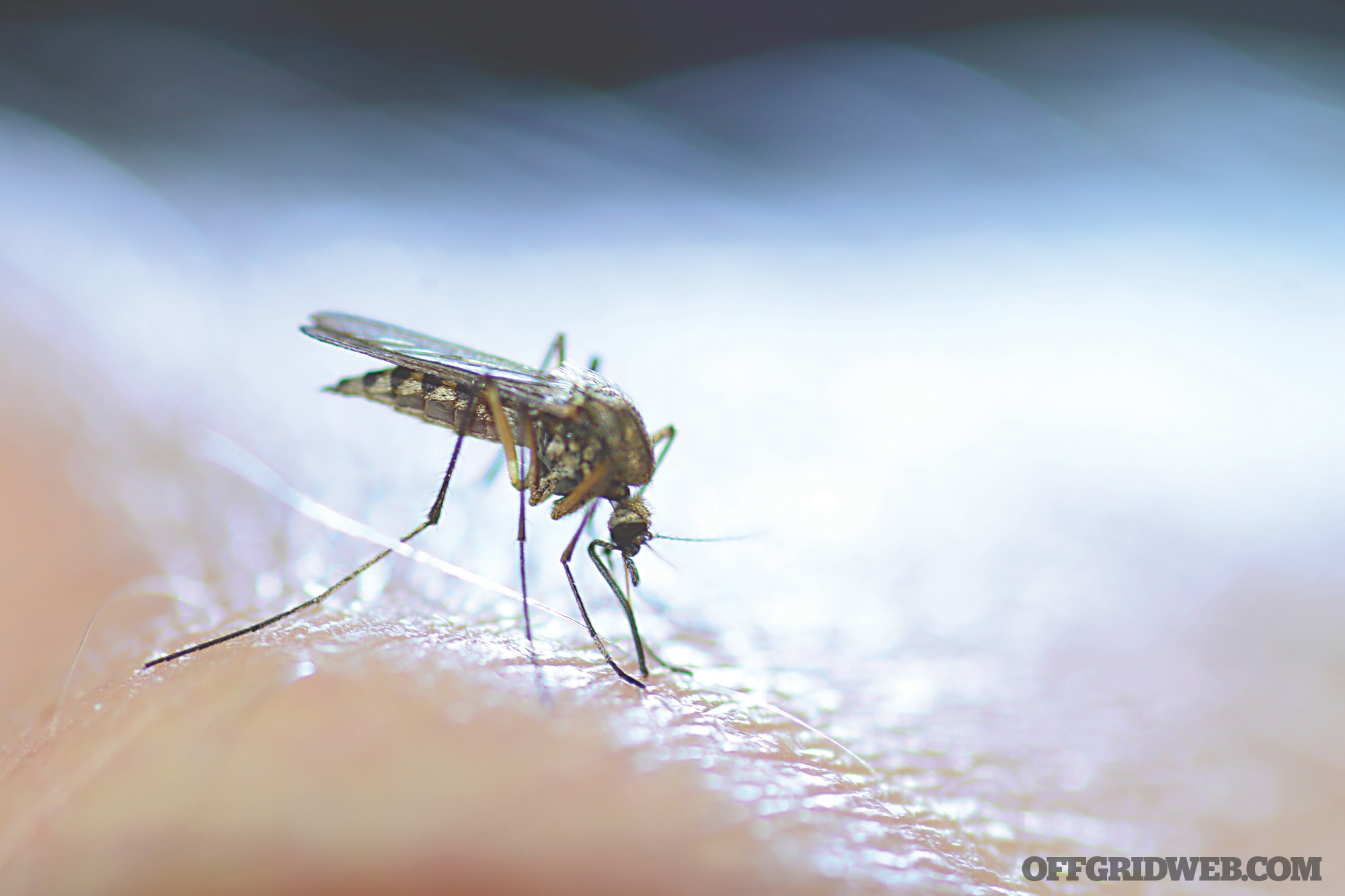
Above: In addition to rodents and hares themselves, mosquitoes can also spread tularemia.
A relatively small number of the bacteria can cause zoonotic diseases, and tularemia is therefore among the list of pathogens that anti-terrorism entities are watching as a potential biological weapon. It can be grown relatively cheaply and easily in a laboratory and is capable of infecting a large population if the bacteria is dispersed via aerosols or other means.
Plague
One of the zoonotic diseases earmarked in human history is plague, but despite its dark reputation, human death by plague is quite rare in the U.S. today. It’s as dangerous as ever, but early diagnosis and treatment normally results in full recovery, as plague can be combatted with commonly available antibiotics.
“Nearly every year, we see large mortality events in wild rodents — prairie dogs and ground squirrels, primarily,” says Dr. Tonie Rocke, a research epidemiologist with the USGS National Wildlife Health Center in Madison, Wisconsin, “but human cases are rare: 5 to 10 a year — 15 cases in a bad year.”
Humans can contract this bacterial disease through direct contact with infected animals, but the more common means of transmission is via flea bites. Once transmitted in this way, a patient will begin to exhibit symptoms in less than a week.
“One common route of transmission to humans in recent years,” explains Rocke, “is via their pets (mostly cats but occasionally dogs) that contract the disease after consuming or contacting an infected rodent. The disease can then be transmitted to their owners either via flea bites or close contact.”
Human symptoms of plague can include fever, chills, headache, weakness, and swollen and tender lymph nodes. The tissue on extremities may turn black and die. If infection reaches the lungs, pneumonia can result.
Diagnosing plague isn’t always easy, unless the patient remembers a flea bite or displays the telltale swollen and painful lymph glands (known as buboes), but chances for successful treatment are good once the disease is confirmed.
Setting Boundaries for Zoonotic Diseases
One point of connection between many of these zoonotic diseases and humans are the four-legged members of our families. Dogs and cats can tangle with infected wildlife and then carry pathogens right into your lap.
Above: Old barns and sheds can harbor rodents and any zoonotic diseases they may carry.
Always note any unexplained changes in your pets or livestock — physical or behavioral. Keep vaccinations up to date. As difficult as it may be to accept, keep in mind that saliva from your pets can carry pathogens, so consider limiting “kisses” from Old Roy.
Similar precautions would apply to livestock, and it’s worth noting that “behavioral changes” can be as telling as the behavior itself. For instance, in the case of rabies, livestock can display either the “furious form” or the “dumb form.” The former is marked by aggression, while the latter manifests as uncharacteristically calm, unafraid, or even friendly behavior.
Zoonotic diseases don’t fit well into SHTF, world-ending narratives. They’re rarely capable of human-to-human transmission beyond a few isolated cases, and they’re relatively easy to avoid with a few common-sense precautions. However, if you live or hunt or farm where wildlife roam, you’re on the front lines, and it pays to be vigilant in protecting yourself and loved ones.
About the Author
Phillip Meeks is an agriculture and natural resources educator originally from Tennessee, but now based in the mountains of Southwest Virginia. He likes to spend his weekends hiking, gardening, beekeeping, fishing, and mushroom hunting.
Related Posts
- What If An Outbreak of Weaponized Pneumonic Plague Hits Your City?
- Condition Red: Avoiding Illness and Disease While Traveling
- HAZE Aerosol Deer Attractant
- Coronavirus: How Concerned Should We Be?
- Jonathan Yoder